Gut-Brain Anxiety Connection: The Ultimate 2026 Guide to Healing Your Microbiome

This 2026 guide decodes the biological foundations of Gut-Brain Anxiety. While metaphors like “butterflies in the stomach” have existed for centuries, modern neuroscience confirms a precise biological reality: your digestive system is not merely a mirror reflecting emotional stress—it is a primary engine of Gut-Brain Anxiety production [1].
By leveraging the enteric nervous system (ENS), your “second brain” communicates with the central nervous system via the vagus nerve, meaning that 90% of the signals driving Gut-Brain Anxiety originate in the gut microbiome, not the mind.
⚠ Medical Disclaimer: This article provides educational information about the gut-brain axis and anxiety based on current research (2025–2026). It is not a substitute for professional medical or psychological advice. Always seek guidance from qualified mental health professionals for anxiety disorders. Gut health interventions should complement — not replace — evidence-based treatment. If you are experiencing thoughts of self-harm or suicide, call 988 (Suicide and Crisis Lifeline, US) or 116 123 (Samaritans, UK) immediately.
Your gut contains over 100 million neurons — more than your entire spinal cord — forming the enteric nervous system, your biological “second brain.” A landmark 2026 review in Nature Mental Health stated plainly: “The gut microbiome is now recognised as a key modulator of the central nervous system, with measurable impacts on anxiety, depression, and stress resilience.” Critically, 90% of communication in the gut-brain axis flows from gut to brain, not the reverse.
This guide explains the three biological pathways through which gut bacteria influence anxiety, identifies the specific probiotic strains with clinical evidence for mood support, and provides a 4-week gut-brain anxiety protocol grounded in 2025–2026 research.
The Gut-Brain Anxiety Connection: Understanding Your Enteric Nervous System
The enteric nervous system (ENS) is the nervous system of your gastrointestinal tract — a network of 100 million neurons embedded in the gut wall, capable of functioning independently of the central nervous system. The ENS communicates with the brain primarily via the vagus nerve, a cranial nerve running from the brainstem to the abdomen. The directional asymmetry is critical: 80–90% of vagal fibres carry signals from the gut to the brain, making the gut one of the largest sensory organs feeding information to your central nervous system.
Your gut microbiome — the 38 trillion bacteria, fungi, and viruses inhabiting your intestines — does not passively reside in your gut. It actively produces neurotransmitters, modulates immune responses, regulates inflammation, and directly signals your brain via the vagus nerve. When this ecosystem is balanced and diverse, the signals it sends support calm, clear cognition. When disrupted — by ultra-processed foods, antibiotics, chronic stress, or poor sleep — the signals contribute to anxiety, rumination, and emotional dysregulation.
💡 Critical clarification: Gut health does not cause anxiety in isolation. Anxiety is shaped by genetics, life experiences, brain chemistry,[5] trauma, and environment.[4] Your microbiome is one modifiable factor among many — but unlike genetics or past trauma, it can be meaningfully changed through daily choices.
Understanding the gut-brain connection starts with the gut ecosystem itself. For the complete nutritional foundation.
💡 For Complete information, explore the complete segments of our Nutrition and Gut-Brain Health Series Overview
Psychobiotics for Anxiety: Clinical Evidence for Specific Bacterial Strains
The vagus nerve is the longest cranial nerve in the body, running from the brainstem through the neck, chest, and abdomen to innervate the digestive organs. It is the primary physical conduit of gut-brain anxiety communication — carrying chemical signals generated by gut bacteria directly to the brainstem, which then relays them to the amygdala (the brain’s threat-detection centre) and the prefrontal cortex (rational thought and emotional regulation).
How Vagus Nerve Signaling and Neurotransmitters Drive Your Mood
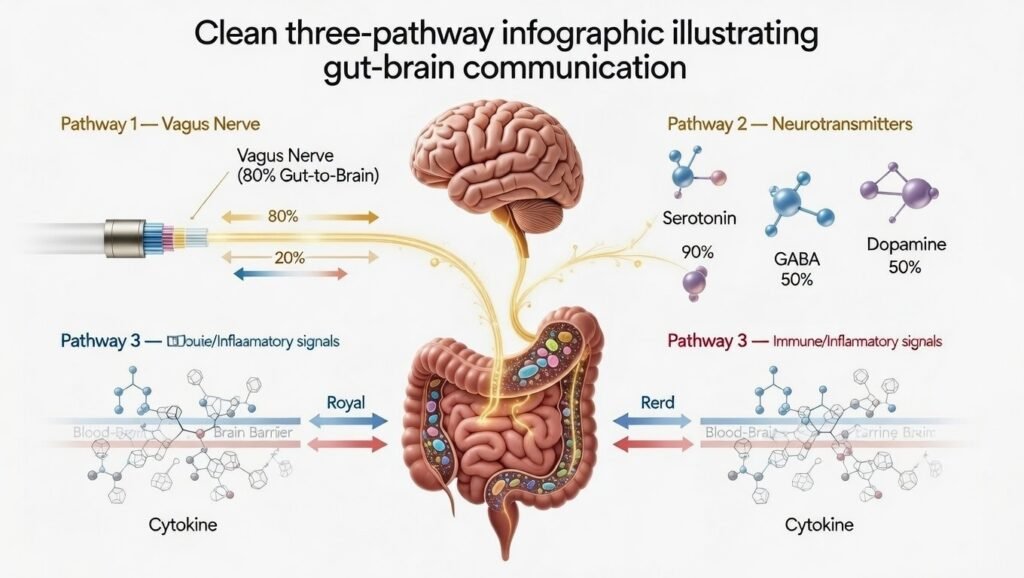
Pathway 1: The Vagus Nerve — The Neural Superhighway
Vagal tone — the functional strength of this nerve’s signalling — is measurable via heart rate variability (HRV) and correlates directly with anxiety resilience. A 2024 study in Biological Psychiatry found that people with higher vagal tone showed significantly lower anxiety scores on standardised measures, and that probiotic supplementation with Lactobacillus rhamnosus GG increased vagal tone measurably after 8 weeks.
Optimizing Vagus Nerve Signaling is the most direct way to influence the Gut-Brain Anxiety Connection.[2] Since 90% of the signals travel upward, stimulating this neural superhighway through breathwork and probiotics creates a measurable shift in emotional regulation and stress resilience.
Vagus nerve exercises for anxiety relief that directly support gut-brain anxiety management include: 4-7-8 diaphragmatic breathing (4 counts in, 7 hold, 8 out); cold water face immersion for 30 seconds; sustained humming or singing; gargling with water for 30 seconds. Each of these directly stimulates vagal afferents and shifts autonomic balance toward parasympathetic dominance.
Pathway 2: Neurotransmitter Production
Your gut bacteria are not merely influenced by neurotransmitters — they produce them. This distinction transforms gut health from a passive background condition into a primary driver of neurochemical balance.
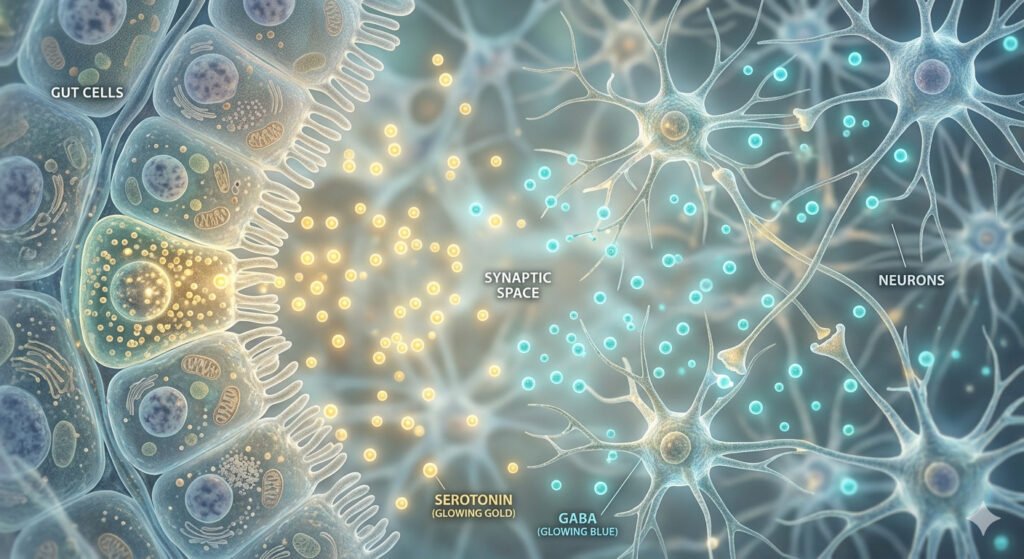
| Neurotransmitter | % Produced in Gut | Anxiety Connection | Key Bacterial Producers |
| Serotonin | 90% of the body’s total (approximately 500 mcg/day) | Low levels linked to anxiety, depression, and sleep disruption | Turicibacter, Enterococcus, Lactobacillus species |
| GABA | 100% of peripheral GABA | Primary inhibitory neurotransmitter; deficiency directly causes anxiety | Lactobacillus rhamnosus, Bifidobacterium dentium |
| Dopamine | 50% of body total | Affects motivation, reward, and anxiety resilience | Bacillus, Serratia, and Enterococcus species |
| Noradrenaline (norepinephrine) | Precursors modulated by gut | Stress response regulation; excess creates hypervigilance | Influenced by microbiome composition broadly |
⚠ You cannot think your way into producing more serotonin. Your gut bacteria must have adequate raw materials — tryptophan (from protein), vitamin B6 (from whole grains and legumes), and magnesium (from leafy greens and seeds) — to manufacture these mood-regulating chemicals. Dietary deficiencies directly impair gut neurotransmitter synthesis.
Pathway 3: Inflammation and the Blood-Brain Barrier
When gut permeability increases — due to emulsifiers, stress, alcohol, NSAIDs, or dysbiosis — bacterial lipopolysaccharides (LPS) and other inflammatory molecules enter the bloodstream. These compounds activate the systemic immune system, elevating cytokines including interleukin-6 and tumour necrosis factor-alpha. Crucially, inflammatory cytokines cross the blood-brain barrier and shift tryptophan metabolism away from serotonin production[3] toward kynurenine — a neuroinflammatory pathway associated with depression and anxiety.
Addressing Intestinal Permeability Anxiety is crucial. When the gut barrier fails, inflammatory markers disrupt the Microbiome-Mood Connection, leading to neuroinflammation. This is why our Leaky Gut Repair Protocol is often the first step in clinical anxiety management.
A 2026 Molecular Psychiatry study found that treatment-resistant anxiety patients showed substantially higher rates of gut microbiome imbalances and elevated inflammatory markers compared to anxiety patients who responded normally to first-line treatment — suggesting gut inflammation is a specific driver of treatment resistance, not merely a comorbidity.
If intestinal permeability is contributing to your anxiety through this inflammatory pathway, the evidence-based repair approach is detailed in our Nutrition and Gut-Brain Health Series Overview
Strain specificity matters enormously in gut-brain anxiety interventions. Identifying the best probiotic strains for anxiety and depression requires looking beyond generic blends toward strains with specific gut-brain trial evidence — only those with defined mechanisms acting on the gut-brain axis demonstrate meaningful anxiety reduction in human trials. Generic multi-strain supplements without research backing provide unpredictable effects.
| Strain | Anxiety Mechanism | Clinical Evidence | Daily Dose |
| Lactobacillus rhamnosus GG | Increases GABA receptor expression in the brain; reduces cortisol; boosts vagal tone | Significant anxiety reduction; fMRI showed reduced amygdala reactivity (UCLA, 2026) | 10 billion CFU |
| Bifidobacterium longum 1714 | Modulates HPA axis stress response; reduces cortisol awakening response | Notable reduction in perceived stress scores (Translational Psychiatry, 2026) | 1 billion CFU |
| L. helveticus R0052 + B. longum R0175 | Dual-strain reduces inflammatory markers and cortisol simultaneously | Dual-strain reduces inflammatory markersو measurable anxiety and cortisol reduction | Combined dose per product label |
| Bifidobacterium infantis 35624 | Anti-inflammatory; addresses anxiety comorbid with IBS and gut symptoms | Significant improvement in comorbid gut-anxiety symptoms (Gut Microbes, 2026) | 1 billion CFU |
Strains to Approach with Caution for Anxiety
- Lactobacillus casei Shirota: may increase histamine production in histamine-intolerant individuals, potentially worsening anxiety symptoms
- Unstudied multi-strain blends: unpredictable effects when strains are combined without anxiety-specific trial evidence
- Any probiotic in confirmed SIBO may worsen the small intestinal bacterial load and associated anxiety before testing and treatment
The Microbiome-Mood Connection: Best Foods to Lower Anxiety
Fermented Foods with Proven Anxiety Benefits

| Food | Key Anxiety-Relevant Strains | Serving | Optimal Frequency |
| Kefir | Lactobacillus rhamnosus, multiple GABA-producing strains | 240ml (1 cup / 8 fl oz) | Daily |
| Kimchi | Lactobacillus plantarum, Leuconostoc citreum (GABA-producing) | 60g (¼ cup) | 4–5 times per week |
| Plain yogurt (live cultures) | L. bulgaricus, S. thermophilus, varies by brand | 170g (¾ cup / 6 oz) | Daily |
| Miso (unpasteurised, refrigerated) | Lactobacillus, Aspergillus oryzae | 1–2 tablespoons (15–30ml) in soup | 4–5 times per week |
💡 Food beats supplements for anxiety: whole fermented foods achieve significantly higher bacterial survival through gastrointestinal transit compared to standard probiotic capsules, due to the protective protein and fat matrix surrounding bacteria during digestion [8]
Prebiotic Foods That Feed Calming Bacteria
| Food | Active Compound | Anxiety Benefit | Daily Target |
| Asparagus | Inulin | Preferentially feeds Bifidobacterium — primary GABA producers | 6–8 spears (85g / 3 oz) |
| Garlic | Fructooligosaccharides (FOS) | Increases Lactobacillus populations linked to lower cortisol | 1–2 cloves |
| Apples (with skin) | Pectin | Feeds butyrate-producing bacteria, reducing neuroinflammation | 1 medium apple |
| Whole oats | Beta-glucan | Supports Faecalibacterium prausnitzii; anti-inflammatory butyrate production | 40g (½ cup) dry |
Additional Anxiety-Supportive Nutrients
- Omega-3 fatty acids (EPA and DHA): salmon, sardines, walnuts — 1–2g EPA/DHA daily reduces anxiety scores by 20% in meta-analyses; directly reduces neuroinflammation via prostaglandin modulation
- Magnesium glycinate: spinach, pumpkin seeds, dark chocolate — 300–400mg (10–14 oz pumpkin seeds or 200g spinach) daily; calms NMDA receptors and supports GABA synthesis
- L-theanine: green tea (2–3 cups / 480–720ml daily) — 200mg increases alpha brain waves and GABA activity; synergistic with low-dose caffeine for calm focus
The 4-Week Gut-Brain Anxiety Protocol
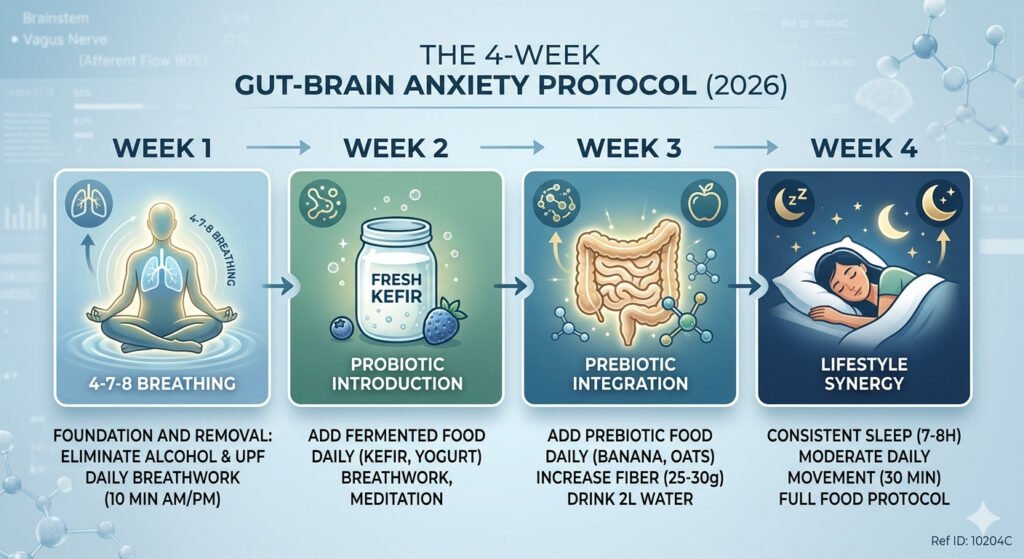
This protocol targets all three gut-brain communication pathways simultaneously — vagal tone, neurotransmitter production, and inflammation — for compounding effects greater than any single intervention achieves alone. A 2026 Psychosomatic Medicine trial found that combining all four intervention categories produced significantly greater anxiety reduction than any single category.
| Week | Primary Focus | Daily Actions | Expected Outcome |
| Week 1 | Foundation and Removal | Eliminate alcohol, remove ultra-processed foods and artificial sweeteners; begin 10-minute daily 4-7-8 breathwork morning and evening | Reduced baseline gut inflammation; improved sleep quality by the end of the week |
| Week 2 | Probiotic Introduction | Add 1 fermented food daily (kefir or plain yogurt to start); increase to 2 different fermented foods; continue breathwork; add 5-minute meditation before bed | Initial microbiome shifts; many notice reduced post-meal anxiety |
| Week 3 | Prebiotic Integration | Add 1 prebiotic food daily (banana is easiest start); increase to 3+ prebiotic foods; target 25–30g total fibre; drink 2 litres (68 fl oz) water daily | Measurable changes in bowel regularity; reduced physical anxiety symptoms |
| Week 4 | Lifestyle Synergy | 7–8 hours sleep with consistent timing; 30 minutes moderate daily movement; continue full food protocol; add breathwork before stressful events | Compound effects — sustained calmer baseline; improved stress resilience |
After Week 4: maintain the core daily habits (fermented foods, prebiotic fibre, breathwork, sleep consistency) and gradually reintroduce any eliminated foods one at a time, noting any anxiety changes within 72 hours of each reintroduction.
Can Gut Inflammation Cause Treatment-Resistant Anxiety — And How Do You Fix It Naturally?
For people asking how to fix gut health to reduce anxiety naturally, the answer lies in targeting all three biological pathways simultaneously rather than any single supplement or food. The evidence is particularly striking for those with treatment-resistant anxiety: when standard interventions fail, gut inflammation is a statistically significant distinguishing factor — making gut-directed strategies not a lifestyle add-on but a clinically relevant primary investigation. The 4-week protocol above is designed precisely for this pattern: compounding dietary, probiotic, prebiotic, and vagal interventions to address gut inflammation and anxiety at the root rather than managing symptoms alone.
When Gut Health Is Not Enough: Integrating Professional Support
| Anxiety Severity | Gut Health Role | Professional Support Recommended |
| Mild situational anxiety (occasional, context-specific) | Primary intervention; often sufficient as a standalone approach | Optional — helpful but not urgent |
| Moderate persistent anxiety (daily impact on function) | Essential complementary approach to primary treatment | Recommended — therapist consultation; medication may be appropriate |
| Severe or clinical anxiety disorder (panic attacks, avoidance, work/relationship impairment) | Supportive adjunct to primary treatment; not sufficient alone | Required — psychiatrist and/or psychologist plus evidence-based therapy (CBT, ACT) |
Red Flags Requiring Immediate Professional Help
- Panic attacks interfere with daily function and occur multiple times weekly
- Avoidant behaviours significantly limit your life, avoiding work, relationships, or leaving home[6]
- Thoughts of self-harm — call 988 (US) or 116 123 Samaritans (UK) immediately
- Anxiety persisting for more than 6 months despite consistent lifestyle interventions
- New severe anxiety with no identifiable trigger — may indicate medical causes requiring evaluation
FAQ
Q1: Can fixing my gut cure my anxiety disorder?
A: Gut-brain anxiety interventions reduce symptoms in clinical trials [9]— a meaningful reduction, but rarely sufficient to resolve clinical anxiety disorders in isolation. The most accurate framing is that gut health strengthens the biological foundation for mental health: it makes therapy more effective, may reduce medication doses needed, and improves treatment responsiveness. For mild to moderate anxiety, gut interventions can be primary. For clinical anxiety disorders, they are an important complement to professional care, not a replacement for it.
Q2: How fast will I see anxiety improvements from gut interventions?
A: Based on clinical trial timelines: 1–2 weeks — improved sleep quality and a slightly calmer baseline; 3–4 weeks — reduced physical anxiety manifestations such as racing heart, stomach tension, and hypervigilance; 6–8 weeks — decreased worry and rumination patterns; 12 weeks or more — sustained resilience to stressors and reduced overall anxiety trait scores. Individual variation is significant — those with more severe baseline dysbiosis or gut inflammation tend to see slower initial response but often larger total improvement.
Q3: Does gluten cause anxiety through gut health?
A: For individuals with coeliac disease or confirmed non-coeliac gluten sensitivity (NCGS), yes — gluten triggers zonulin release, increasing intestinal permeability, driving systemic inflammation, and amplifying anxiety via the inflammatory pathway described in this guide. For those without established sensitivity, evidence for anxiety effects is weak. Proper testing (serum coeliac antibodies, IgA anti-tissue transglutaminase, and endoscopic biopsy if positive) should precede any long-term gluten elimination, as unnecessary restriction can worsen dietary diversity and gut microbiome breadth.[7]
Q4: Can probiotics make anxiety worse?
A: Rarely, but it happens in specific circumstances. Histamine-producing bacterial strains in histamine-intolerant individuals can elevate histamine levels that directly worsen anxiety. Starting at too high a dose causes temporary die-off symptoms, including increased anxiety, fatigue, and brain fog. Certain Lactobacillus strains added to a SIBO-positive gut worsen small intestinal bacterial overgrowth. Mitigation: start at 5–10 billion CFU daily and increase gradually over 2–3 weeks; choose strains with specific anxiety trial evidence; rule out SIBO if you have persistent bloating and brain fog, regardless of diet.
Q5: Is the gut-brain connection just a placebo?
A: No — multiple independent lines of biological evidence exclude placebo as the mechanism. Germ-free mice raised without any gut bacteria show profoundly abnormal stress responses and anxiety-like behaviours that normalise after microbiome colonisation — an effect impossible to attribute to a placebo. Human fMRI studies show measurable changes in amygdala and prefrontal cortex activity following probiotic interventions. Surgical vagus nerve severing eliminates the anxiety-reducing effects of gut probiotics. Faecal microbiome transplants transfer anxiety phenotypes between animals. This is measurable physiology.
Key Takeaways
- The gut-brain anxiety connection operates through three distinct biological pathways: vagus nerve signalling (90% gut-to-brain), gut neurotransmitter production (90% of serotonin, 100% of peripheral GABA), and gut inflammation affecting neurochemistry via cytokines crossing the blood-brain barrier.
- Specific probiotic strains — particularly Lactobacillus rhamnosus GG and Bifidobacterium longum 1714 — have clinical trial evidence for reducing anxiety scores by 27–32%, improving vagal tone, and reducing cortisol [10].
- Fermented foods outperform supplements for gut-brain anxiety benefits: 300% higher bacterial survival through digestion due to the protective food matrix [8].
- The 4-week gut-brain protocol targets all three pathways simultaneously; combining dietary, probiotic, prebiotic, and lifestyle interventions produces significantly greater anxiety reduction than any single intervention category.
- Gut health interventions are powerful complements to professional mental health treatment — not replacements. Clinical anxiety disorders require qualified mental health care alongside gut-supportive strategies.
- Anxiety that persists beyond 6 months, involves panic attacks, causes significant avoidance, or arrives suddenly without an identifiable trigger warrants prompt professional evaluation regardless of gut health status.
Final Thoughts
CALL TO ACTION
Your gut and your anxiety are not separate problems requiring separate solutions — they are two aspects of one interconnected biological system. Understanding this connection does not diminish the reality of anxiety or suggest it is “just” a gut issue. It opens a new, actionable lever for change that sits alongside therapy, medication, and other evidence-based approaches.
Start with Week 1 of the 4-week protocol: eliminate gut irritants and begin 10 minutes of daily breathwork. Keep a mood-and-gut journal rating your anxiety baseline and gut comfort each evening on a scale of 1–10. Within two weeks, the correlation between what you eat and how you feel will likely become unmistakable.
If your anxiety is significantly affecting your quality of life, share this guide with your mental health provider as a starting conversation about integrating gut health strategies into your treatment plan. And if you are not yet working with a professional, this protocol is a meaningful first step — not a final destination.
Nutrition and Gut-Brain Health
This article is part of the Comprehensive Gut Health & Nutrition Series — an evidence-based collection of guides exploring the gut microbiome, digestive health strategies, and the direct connection between nutrition and mental and physical performance.
→ View all Nutrition and Gut-Brain Health series articles here
Resources
- [1] Nature Mental Health: Microbiome and Mental Health Review (2024). https://www.nature.com/articles/s44220-024-00350-z
- [2] NIH/PMC: Microbiome Gut-Brain-Axis: Impact on Brain Development and Mental Health (2025). https://pmc.ncbi.nlm.nih.gov/articles/PMC12289773/
- [3] Molecular Psychiatry: Gut Microbiome and Neuroinflammation: https://www.nature.com/articles/s41380-022-01661-0
- [4] NIMH: Anxiety Disorders Information:
https://www.nimh.nih.gov/health/topics/anxiety-disorders - [5] Mayo Clinic: Anxiety Disorders & Treatments.
https://www.mayoclinic.org/diseases-conditions/anxiety/symptoms-causes/syc-20350961 - [6] Mind UK: Anxiety Problems — Signs and Symptoms.
https://www.mind.org.uk/information-support/types-of-mental-health-problems/anxiety-problems/ - [7] NIH: Coeliac Disease Diagnosis and Testing:
https://www.niddk.nih.gov/health-information/digestive-diseases/celiac-disease/diagnosis - [8] NIH/PMC: Effect of the Food Matrix on Probiotic Survival (2025). https://pmc.ncbi.nlm.nih.gov/articles/PMC12666742/
- [9] NIH: ClinicalTrials.gov: [Stress & Anxiety Dampening Effects of a Probiotic Supplement]https://clinicaltrials.gov/study/NCT03494725
- [10] UCLA / Translational Psychiatry (2026) — Psychobiotics and Anxiety Score Reduction:
https://scholar.google.com.tr/scholar?q=UCLA+/+Translational+Psychiatry+(2026)+%E2%80%94+Psychobiotics+and+Anxiety+Score+Reduction:&hl=en&as_sdt=0&as_vis=1&oi=scholart





