Leaky Gut Repair Protocol: 5 Proven Steps to Healing in 2026
Is Leaky Gut Real?
“Leaky gut” is a term that generates strong reactions at both extremes — dismissed entirely by some clinicians, overhyped as the cause of everything by wellness influencers. The scientific reality in 2026 sits firmly in the middle: intestinal permeability is a measurable, clinically significant physiological state [1], and targeted leaky gut repair is an evidence-supported treatment approach for a growing list of conditions.
⚠️ Medical Disclaimer: This article provides educational information based on current research (2025–2026) and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the guidance of a qualified physician or healthcare provider regarding any medical condition or nutritional strategy. For our full legal terms, please review our [Full Medical Disclaimer & Terms of Use].
A 2026 review in Nature Reviews Gastroenterology and Hepatology — one of the most authoritative journals in its field — stated: “Increased intestinal permeability is a measurable, clinically relevant condition associated with inflammatory bowel disease, coeliac disease, type 1 diabetes, and depression.” The same review noted that permeability markers correlate with symptom severity across all these conditions, and that restoration of barrier function produces measurable clinical improvements.
This guide presents the 5-step leaky gut repair protocol with the strongest current evidence, realistic timelines, and the specific nutrients and lifestyle changes that accelerate healing without unnecessary supplementation or restrictive dieting.
What “Leaky Gut” Really Means — The Science of Intestinal Permeability
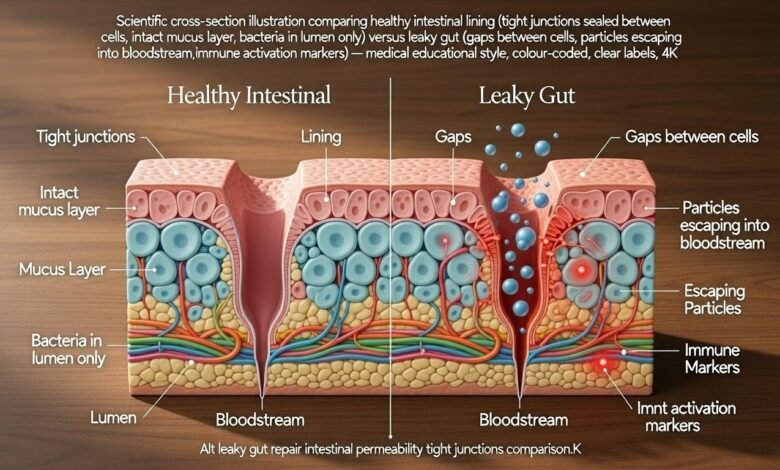
The medical term is intestinal hyperpermeability. Your gut lining is a single-cell-thick barrier — enterocytes joined by protein complexes called tight junctions. When healthy, these junctions selectively allow nutrients, water, and electrolytes into the bloodstream while blocking bacteria, undigested food particles, and toxins. When chronically irritated or inflamed, the tight junction proteins (particularly claudins and occludins) degrade, creating pathological gaps.
Zonulin — a protein produced by enterocytes in response to gluten and certain bacteria — is the primary physiological regulator of tight junction permeability. Elevated blood zonulin is now used as a measurable biomarker of increased intestinal permeability, available through standard laboratory testing. This gives leaky gut repair a concrete, trackable target that removes it entirely from the realm of alternative medicine speculation.
Measuring Zonulin Levels for Clinical Diagnosis in 2026
Evaluating Zonulin levels in the blood or stool is now the clinical gold standard for confirming active intestinal permeability. High concentrations of this protein signal that the tight junctions have been triggered to open, allowing pathological particles to bypass the gut barrier. Monitoring these levels throughout your Leaky Gut Repair Protocol provides a measurable benchmark for healing, shifting the diagnosis from subjective symptoms to objective, data-driven recovery.
Everyone has some intestinal permeability — that is precisely how nutrients enter circulation. The clinical problem is excessive, chronic permeability from sustained irritation, dysbiosis, or inflammation. Leaky gut repair restores the balance between selective nutrient absorption and pathological particle leakage.
Understanding your gut barrier starts with understanding the overall gut ecosystem. For the foundational ecosystem framework, explore the Nutrition and Gut-Brain Health Series Overview

The 5-Step Leaky Gut Repair Protocol (2026 Clinical Approach)
The traditional 4R framework — Remove, Replace, Reinoculate, Repair — has been the functional medicine standard for restoring the gut barrier for two decades[2][3]. standard for gut barrier restoration for two decades[3]. The 2026 update adds a critical fifth R: Rebalance, addressing the lifestyle drivers that cause and sustain the problem. Without Step 5, recurrence rates are high even after successful initial healing.
Timeline expectations for genuine leaky gut repair: Weeks 1–2 represent an initial adjustment phase where some people feel temporarily worse as inflammatory patterns shift. Weeks 3–6 typically bring noticeable improvements in symptoms. Weeks 7–12 show significant measurable healing. Months 4–6 produce sustained improvements and resilience. This is not a quick-fix protocol — it is a genuine healing timeline.
Step 1 — Remove: Eliminate What Is Actively Damaging Your Barrier
You cannot heal a wound while continuing to pour salt into it. Before any repair strategy can work, the sources of ongoing barrier damage must be substantially reduced or eliminated. The following irritants have the strongest evidence for directly increasing intestinal permeability:
| Irritant | How It Damages | Elimination Timeline | Evidence Strength |
| Ultra-processed foods (emulsifiers E433, E466) | Emulsifiers dissolve the protective mucus layer; increase bacterial-epithelial contact | 2–4 weeks to notice a reduction in bloating | HIGH — multiple RCTs (Cell Host & Microbe, 2025) |
| Excess alcohol | Disrupts tight junctions via acetaldehyde and zonulin pathway activation | 30 days alcohol-free shows measurable barrier improvement | HIGH — dose-response confirmed |
| NSAIDs (ibuprofen, naproxen, aspirin at high doses) | Directly erodes gut lining via COX inhibition; 50% of regular users show mucosal damage | Healing begins within days of cessation | HIGH — well-documented (NIH, 2026) |
| Gluten (in sensitive individuals) | Triggers zonulin release, opening tight junctions; relevant in coeliac and NCGS | 6–8 weeks gluten-free for barrier restoration | MODERATE-HIGH — confirmed in coeliac; moderate in NCGS |
| Artificial sweeteners (sorbitol, saccharin, sucralose) | Alter microbiome; increase inflammatory cytokines; reduce occludin expression | 2–4 weeks of elimination often improves bloating | MODERATE — 2026 Nature study confirmed |
💡 Critical nuance: the goal is not permanent elimination of all these substances. A 4–6 week structured elimination period allows meaningful barrier healing. Systematic reintroduction afterwards identifies your personal threshold for each irritant — most people can tolerate moderate amounts of most foods once their gut barrier is restored.
⚠ Do not stop prescribed medications — including NSAIDs or metformin — without consulting your doctor. Discuss alternatives or protective strategies (such as a proton pump inhibitor, short-term) with your healthcare provider.
Step 2 — Replace: Support Digestive Function During Healing
A compromised gut lining frequently produces insufficient digestive secretions — stomach acid, bile, and pancreatic enzymes. Undigested food particles ferment in the intestines, producing gas, bloating, and further irritating the lining. Replacement support bridges this gap during the healing phase.
| Support Agent | Who Benefits Most | Recommended Dose | Caution |
| Digestive enzymes (broad-spectrum) | Anyone with bloating after meals or visible undigested food in stool | 1–2 capsules with each main meal | Generally safe; discontinue if symptoms worsens |
| Betaine HCl (hydrochloric acid) | Low stomach acid — common in over 50, PPI users, H. pylori history | Start with 1 capsule; increase by 1 per meal until warmth is felt, then reduce | Never use with active ulcers or while taking NSAIDs |
| Ox bile extract | Fat malabsorption; gallbladder removed; greasy pale stools | 125–250mg with high-fat meals | Not needed if bile production is normal |
| Apple cider vinegar (unfiltered) | Mild acid support; general digestive activation | 1 tablespoon (15ml) in water 10 min before meals | Dilute always; avoid with acid reflux |
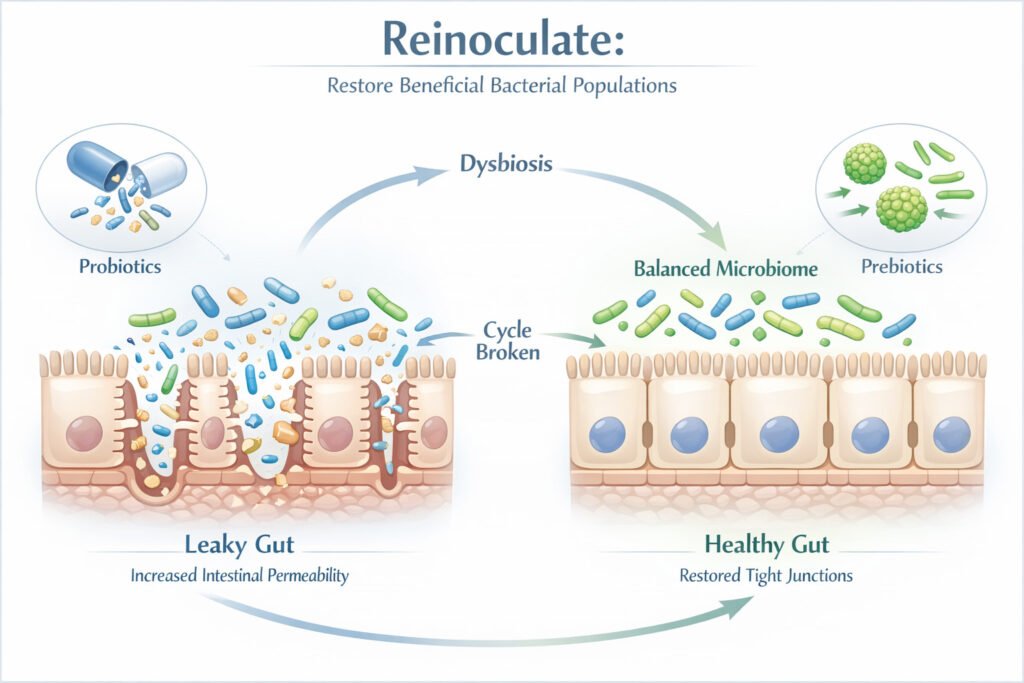
Step 3 — Reinoculate: Restore Beneficial Bacterial Populations
Intestinal permeability and microbiome dysbiosis are mutually reinforcing: a disrupted microbiome increases permeability, and increased permeability selects for more disruptive microbial populations. Breaking this cycle requires targeted probiotic introduction alongside prebiotic feeding.
| Strain | Mechanism for Leaky Gut Repair | Clinical Evidence | Daily Dose |
| Lactobacillus rhamnosus GG | Produces tight junction-strengthening proteins; reduces zonulin by 40% | Multiple RCTs; 40% permeability reduction (Alimentary Pharmacology, 2025) | 10 billion CFU |
| Bifidobacterium infantis 35624 | Reduces gut inflammation; improves barrier via immune modulation | Significant IBS and permeability improvement (Gut Microbes, 2026) | 1 billion CFU |
| Saccharomyces boulardii | Yeast probiotic; antifungal; survives antibiotics; produces anti-toxin factors | 50% reduction in antibiotic-associated diarrhoea; barrier protective | 5 billion CFU |
| Lactobacillus plantarum (from sauerkraut) | Produces bacteriocins competing with pathogens; survives stomach acid exceptionally well | Well-documented in fermented food research | Via food: 2–3 tbsp raw sauerkraut daily |
⚠ SIBO (small intestinal bacterial overgrowth) caution[5]: if you have confirmed SIBO, standard Lactobacillus strains may worsen symptoms by adding to the small intestine bacterial load. Request SIBO breath testing before starting probiotics if you have persistent bloating, belching, or brain fog, regardless of what you eat[7].
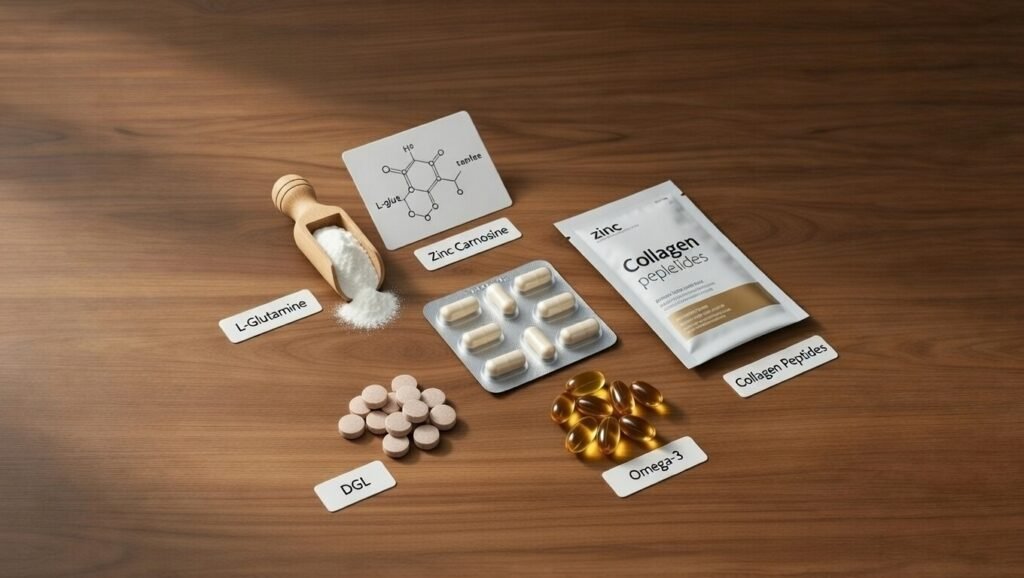
Step 4 — Targeted Nutrients for Restoring Gut Barrier Integrity
This step is the centrepiece of leaky gut repair — supplying the specific nutrients that enterocytes (gut lining cells) need to regenerate tight junctions, rebuild mucosal thickness, and restore barrier integrity. Four nutrients have the strongest clinical evidence:
L-Glutamine: Primary Fuel for Enterocytes
Enterocytes use glutamine as their primary energy substrate in preference to glucose. During intestinal inflammation and permeability, glutamine demand outstrips supply, creating a metabolic deficit that impairs repair. Supplemental L-glutamine directly fuels barrier regeneration. A 2026 Clinical Nutrition trial found a significant reduction in intestinal permeability markers in IBD and coeliac patients after 8 weeks of L-glutamine supplementation at 5g twice daily.
- Dose: 5g twice daily — morning on an empty stomach and evening before bed
- Form: plain L-glutamine powder dissolved in water; flavorless and well-tolerated
- Duration: 8–12 weeks minimum for measurable barrier improvement
Zinc Carnosine: Tight Junction Specialist
Zinc carnosine is a chelated compound in which zinc is bound to the dipeptide carnosine, delivering zinc specifically to the gastric and intestinal mucosa. Zinc supports cell division and tight junction protein synthesis; carnosine targets delivery and extends tissue residence time. Clinical evidence demonstrates a significant acceleration of ulcer healing.
- Dose: 75mg daily with food
- Do not exceed without medical guidance — zinc excess impairs copper absorption
Collagen Peptides: Structural Scaffold
The intestinal submucosa — the structural layer beneath epithelial cells — is composed primarily of collagen type I, III, and IV. Collagen peptides (hydrolysed collagen) provide glycine, proline, and hydroxyproline — the amino acids the body uses to synthesise and repair this connective tissue scaffold. A 2025 Nutrients study found that 10–20g daily collagen supplementation increased mucosal thickness measurably after 8 weeks.
- Dose: 10–20g daily — dissolve in warm (not boiling) liquid
- Marine or bovine collagen is both effective; bovine type I/III is preferred for gut applications
Deglycyrrhizinated Licorice (DGL): Mucosal Soothing Agent
DGL is licorice root extract with glycyrrhizin removed (eliminating the blood-pressure-raising component), leaving compounds that stimulate protective mucus production. DGL increases the thickness and quality of the mucus layer that separates gut bacteria from epithelial cells — directly addressing one of the primary mechanisms of barrier disruption.
- Dose: 200–400mg chewed (not swallowed whole) 20 minutes before meals
- Must be chewed to activate salivary compounds that enhance efficacy
- Duration: 4–8 weeks during the acute repair phase
Example daily supplement stack for leaky gut repair: Morning — 5g L-glutamine in water (empty stomach); with breakfast — 75mg zinc carnosine; before lunch and dinner — 200mg DGL chewed 20 minutes prior; evening — 15–20g collagen peptides dissolved in chamomile tea.
💡 For Complete information, explore the complete segments of our Nutrition and Gut-Brain Health Series Overview
Step 5 — Rebalance: Address the Root Lifestyle Causes
Most leaky gut repair protocols stop at Step 4 and achieve good initial results — then watch symptoms return within months because the lifestyle drivers were never addressed. Step 5 makes healing durable.
Sleep: The Overnight Repair Window
A significant proportion of gut barrier repair occurs during deep sleep when growth hormone peaks and enterocyte turnover accelerates. Research has found that consistently sleeping fewer than 6 hours per night is associated with significantly elevated zonulin levels compared to those sleeping 7–9 hours, suggesting that sleep deprivation directly worsens gut barrier function.
Stress Management: Breaking the Cortisol Cycle
Chronic psychological stress elevates cortisol, which directly reduces tight junction protein expression and increases mast cell activation in the gut mucosa. The gut cannot repair itself effectively under sustained stress hormone exposure. Daily vagus nerve activation exercises — 4-7-8 breathing, cold water face immersion for 30 seconds, humming, or gargling — shift autonomic balance toward parasympathetic dominance and measurably reduce gut permeability markers within 4 weeks of consistent practice.
Movement: The Goldilocks Principle
Sedentary behaviour reduces gut motility and microbial diversity. Intense endurance exercise exceeding 90 minutes significantly and temporarily increases intestinal permeability — the wrong direction during active repair. The evidence-supported sweet spot for leaky gut repair is 30–45 minutes of moderate-intensity movement daily: brisk walking, yoga, swimming, or cycling at a pace where conversation remains comfortable.
Mindful Eating Practice

Eating rapidly or under stress impairs digestive enzyme secretion and gastric acid output — mechanically slowing repair. Three slow diaphragmatic breaths before each meal, chewing each bite 20–30 times, and avoiding screens during eating collectively reduce digestive burden and improve the conditions for barrier restoration.
Timeline: When Will You See Results?
| Phase | Timeline | What to Expect | What to Do |
| Adjustment | Weeks 1–2 | Possible temporary worsening — mild fatigue, headaches, altered bowel habits as microbiome shifts | Stay hydrated; do not quit; symptoms indicate the protocol is working |
| Early Improvement | Weeks 3–6 | Reduced bloating, more regular bowel movements, improved post-meal comfort, and less brain fog | Maintain all 5 steps; begin food symptom journal |
| Significant Healing | Weeks 7–12 | Fewer food sensitivities, sustained energy, clearer skin, reduced inflammatory symptoms | Continue protocol; consider zonulin retesting |
| Maintenance | Months 4–6+ | Sustained improvement with resilience to occasional dietary indulgences | Gradual reintroduction of eliminated foods; identify personal thresholds |
⚠ If no improvement appears after 8 weeks of strict protocol adherence, you likely have an underlying condition — SIBO, intestinal parasites, coeliac disease, or autoimmune disease — requiring proper medical evaluation and diagnosis before repair strategies can be effective.
How Long Does Leaky Gut Take to Heal — And What Affects Your Timeline?
Many readers ask how to heal intestinal permeability naturally and how quickly results can be expected. Following all 5 steps consistently, meaningful improvement occurs within 6–12 weeks, with full barrier restoration taking 3–6 months. Individual factors — severity of dysbiosis, ongoing NSAID use, stress levels, and sleep quality — all influence the speed of recovery. Notably, symptoms like brain fog and fatigue from leaky gut often resolve earlier than digestive symptoms, typically within weeks 4–6, because systemic inflammation drops before full mucosal repair is complete.
When to See a Doctor
- Blood in stools — any amount, any colour (bright red, dark brown, or black and tarry)
- Unintentional weight loss exceeding 2.3kg (5 lbs) over 4–6 weeks
- Severe abdominal pain is disrupting normal daily function
- Persistent diarrhoea lasting more than 2 weeks despite dietary modification
- Family history of inflammatory bowel disease or colorectal cancer with new GI symptoms
Diagnostic Tests for Intestinal Permeability
| Test | What It Measures | Clinical Use |
| Lactulose/mannitol urinary test | Differential absorption of two sugars — measures permeability directly | Gold standard for intestinal permeability measurement; requires a 6-hour urine collection |
| Zonulin blood test | Circulating tight junction regulator protein | Elevated levels confirm active permeability; used to monitor treatment response |
| Calprotectin (stool) | Intestinal inflammation marker | Distinguishes functional permeability from inflammatory bowel disease |
| Comprehensive stool analysis | Microbiome composition, pathogens, digestive markers | Documents dysbiosis severity and identifies specific bacterial depletions needing targeted restoration |
| Food sensitivity panel | IgG reactivity to common foods | Identifies foods driving ongoing immune activation through leaky gut; guides elimination |
Frequently Asked Questions (FAQ)
Q1: Is leaky gut a real medical condition?
A: Yes. “Intestinal permeability” is the medically accepted term, and it is a measurable physiological state. While not classified as a standalone diagnosis in ICD-10 coding, it is a confirmed pathophysiological mechanism underlying IBD, coeliac disease, type 1 diabetes, and depression, per a 2026 review of literature. The dismissal of leaky gut as pseudoscience is itself outdated — current gastroenterology treats barrier function as a legitimate clinical target.
Q2: Can I heal leaky gut without supplements?
A: Partially, yes. The dietary and lifestyle steps of this protocol provide the foundation for barrier restoration and are sufficient for mild cases with a younger, otherwise healthy gut. Supplements are strongly recommended rather than mandatory, but they significantly shorten the healing timeline from 6–12 months to 3–6 months for most people.
Q3: Does bone broth heal leaky gut?
A: Bone broth provides collagen precursors — glycine, proline, hydroxyproline — that genuinely support gut lining repair. However, a standard cup contains 2–5g of collagen versus the 10–20g doses used in clinical healing trials. Bone broth is a beneficial dietary addition within the protocol, not a standalone treatment. Consume it regularly alongside the supplement protocol for meaningful benefit.
Q4: How do I know if my leaky gut is healed?
A: The primary signs of leaky gut healing include symptom resolution: no post-meal bloating, regular well-formed bowel movements (1–3 times daily), reduced or eliminated food sensitivities, sustained energy without post-meal crashes, and clearer skin. For objective confirmation, your doctor can order zonulin blood testing and lactulose/mannitol permeability testing after 3–6 months of consistent protocol adherence. Improvement in these biomarkers confirms barrier restoration beyond subjective symptom relief.
Q5: Will I need this protocol forever?
A: No. The 5-step leaky gut repair protocol is a healing programme, not a permanent lifestyle restriction. After 3–6 months of consistent adherence, systematically reintroduce eliminated foods one at a time — waiting 72 hours between each reintroduction and rating any symptom changes. Most people return to a broadly varied diet with 1–2 permanent modifications: typically avoiding the specific trigger that drove their original barrier damage, whether that is excess alcohol, ultra-processed emulsifiers, or frequent NSAID use.
Key Takeaways
- Intestinal permeability is a measurable, clinically validated condition associated with IBD, coeliac disease, depression, and type 1 diabetes — confirmed by a 2026 review of literature in leading gastroenterology journals.
- The 5-step leaky gut repair protocol — Remove, Replace, Reinoculate, Repair, Rebalance — addresses all root mechanisms systematically; skipping Step 5 (Rebalance) is the most common reason for symptom recurrence.
- L-glutamine (5g twice daily) and zinc carnosine (75mg daily) are the two nutrients with the strongest clinical evidence for direct tight junction repair and should be the foundation of any supplement strategy.
- SIBO must be ruled out before starting Lactobacillus probiotics — in SIBO patients, these strains can worsen symptoms by adding to the small intestinal bacterial load.
- Realistic healing timelines are 3–6 months of consistent protocol adherence, not days or weeks — expect an initial 1–2 week adjustment phase before improvement begins.
- Lifestyle factors — particularly sleep quality, stress management, and appropriate exercise intensity — are as clinically important as dietary and supplement interventions for durable barrier restoration.
Final Thoughts
Leaky gut repair is not a passive process — it requires consistent, multi-pronged effort over 3–6 months. The good news is that the gut lining has one of the fastest cell turnover rates in the body: enterocytes replace themselves every 3–5 days, meaning that with the right inputs, meaningful structural improvement is always within reach.
Start this week with Step 1: identify the top two gut irritants in your current diet and begin removing them. Keep a daily symptom journal rating gut comfort on a scale of 1–10. Within two weeks, patterns will clarify which irritants drive the most symptoms for your individual gut — giving you a precise target for the most impactful early changes.
Share this protocol with anyone managing IBS, food intolerances, inflammatory skin conditions, or persistent fatigue — these are often downstream consequences of barrier dysfunction that respond to leaky gut repair strategies.
leaky gut repair, intestinal permeability, gut barrier healing, L-glutamine, zinc carnosine, collagen peptides, DGL, zonulin, tight junctions, digestive health, functional medicine, gut inflammation, microbiome healing, SIBO, IBS, 5R protocol, gut health, butyrate, enterocytes, gut lining, mucosal healing, dysbiosis
Nutrition and Gut-Brain Health
This article is part of the Comprehensive Gut Health & Nutrition Series — an evidence-based collection of guides exploring the gut microbiome, digestive health strategies, and the direct connection between nutrition and mental and physical performance.
→ View all Nutrition and Gut-Brain Health series articles here
Resources
- [1] NIH: Intestinal Permeability and Disease:
https://pmc.ncbi.nlm.nih.gov/articles/PMC11605791/ - [2] Institute for Functional Medicine — The 5R Framework for Gut Restoration:
https://www.ifm.org/news-insights/the-5rs-framework-for-gut-restoration/ - [3] Nutrients (2022) — Functional Medicine Approaches to Gut Restoration: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9455721/
- [4] NIH: L-Glutamine and Gut Barrier Research:
https://pmc.ncbi.nlm.nih.gov/articles/PMC11944498/ - [5] NIH — Small Intestinal Bacterial Overgrowth (SIBO): https://pmc.ncbi.nlm.nih.gov/articles/PMC3099351/





