Men’s Mental Health Unmasked: Breaking The Silence to Sustainable Strength

The Silent Epidemic: Understanding Men’s Mental Health Statistics
Men’s mental health is often overlooked or misunderstood, leaving many to struggle in silence due to societal pressures. Although depression and anxiety affect men as much as women, the unique challenges of men’s mental health require a specialized approach to early recognition and support. This article highlights these hidden struggles and provides practical steps for building sustainable emotional resilience [1].
⚠️ Medical Disclaimer: This article provides educational information about men’s mental health based on research (2025–2026) and is not a substitute for professional medical advice. Always consult a licensed therapist or healthcare provider for mental health concerns.
The statistics reveal a devastating picture that demands immediate attention:
- According to CDC latest research on Men’s Mental Health, men account for the majority of suicide[9] deaths in the United States, with suicide rates several times higher than those of women. [1]
- Approximately 40% of men with a mental illness receive treatment, compared to about 52% of women. [2]
- Research suggests men are significantly less likely to seek timely mental health support compared to women [3]–[4], often delaying care until symptoms become severe.
- Approximately one in five adults experiences a mental health condition each year. [11] —yet most suffer in silence
- Male caregivers often face unique emotional burdens, particularly when supporting loved ones with chronic conditions.[4]
These are fathers who never saw their children graduate, brothers who disappeared from family gatherings, and sons who stopped returning calls. The cost of silence extends far beyond individual suffering—it fractures families, devastates workplaces, and leaves communities grieving preventable losses.
The turning point: Recognizing that emotional suppression isn’t strength—it’s a learned behavior reinforced since childhood that can be unlearned with conscious effort and safe support.
Why Men Stay Silent: Deconstructing the “Strong Man” Myth
Breaking the silence is the first step toward improving men’s mental health. The “Strong Man” myth often forces men to suppress emotions, creating a significant barrier to men’s mental health recovery and sustainable emotional resilience.
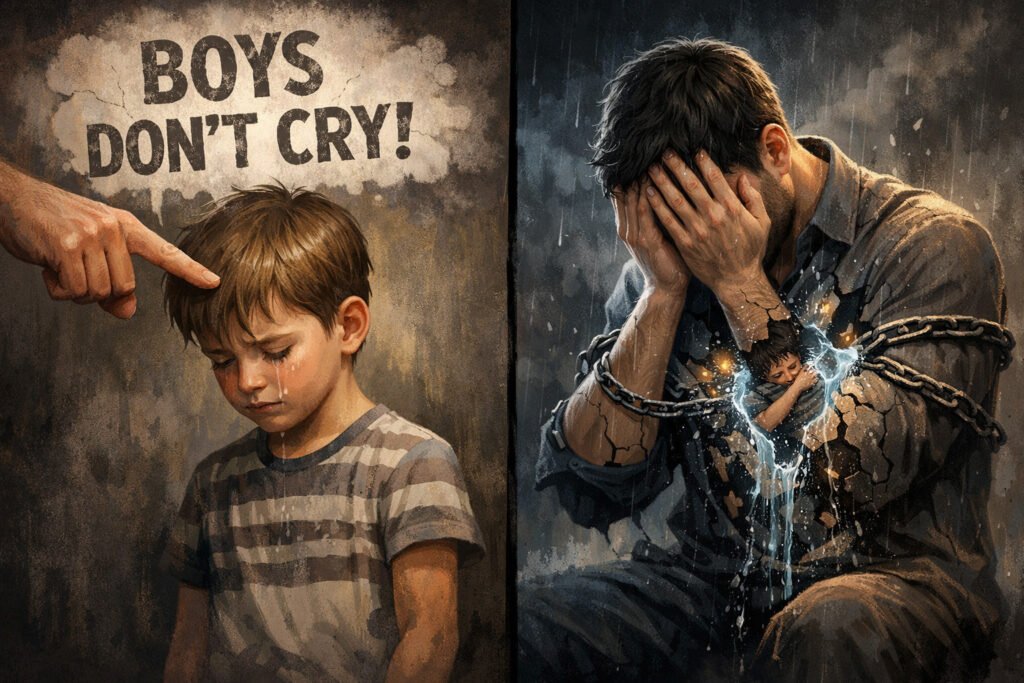
From playground to boardroom, men receive consistent, reinforcing messages about emotional expression. Childhood conditioning teaches boys that vulnerability equals weakness—a lesson absorbed before critical thinking fully develops. Media reinforcement portrays male heroes as emotionally detached. Workplace culture rewards grinding through stress without complaint.
This conditioning doesn’t eliminate emotions—it redirects them into more “acceptable” male expressions that often harm relationships and health:
| Suppressed Emotion | Common Male Expression | Long-Term Consequence |
| Sadness | Anger, irritability, withdrawal from relationships | Damaged relationships; elevated cardiovascular strain |
| Fear | Risk-taking, substance use, workaholism | Accidents; addiction; progressive burnout |
| Vulnerability | Emotional numbness, detachment from others | Loneliness; inability to form deep bonds |
| Anxiety | Perfectionism, control issues, harsh criticism | Chronic stress, relationship conflict, and health decline |
Studies have linked chronic emotional suppression in men with increased cardiovascular risk, substance misuse, and occupational stress outcomes. [3][4]
The paradigm shift: True strength isn’t the absence of struggle—it’s the courage to acknowledge difficulty and seek support while continuing to move forward. The strongest men aren’t those who never fall; they’re those who get back up, ask for help when needed, and keep going.
Male-Pattern Symptoms: How Men’s Mental Health Issues Manifest Differently
Understanding how symptoms differ is crucial for men’s mental health advocacy. Instead of typical sadness, men’s mental health struggles often manifest as irritability, risk-taking, or escapism through work or substance use.
Men often don’t present with classic depression symptoms like persistent sadness, crying, or verbalizing hopelessness. Instead, watch for these male-pattern indicators that frequently get dismissed or mislabeled:
Behavioral Warning Signs
| Sign | What It Looks Like | Why It’s Overlooked |
| Irritability / Anger | Snapping at family over minor issues, road rage, and workplace conflicts | “That’s just his personality,” or “He’s stressed at work. “ |
| Withdrawal | Excessive time alone in the garage or workshop, avoiding social events | “He needs his space,” or “Men are just less social,” |
| Risk-taking | Reckless driving, dangerous hobbies, financial gambles | “Midlife crisis” or “He’s just being impulsive. “ |
| Substance use | Daily drinking to “unwind,” prescription misuse, weekend binges | “Everyone does it.” or “It’s just how he relaxes.” |
| Work obsession | 70+ hour weeks, never taking a vacation, worth tied to productivity | “He’s dedicated” or “A good provider.” |
Emotional & Cognitive Warning Signs
- Emotional numbness: “I don’t feel anything anymore”—not sadness, but emptiness or flatness
- Loss of interest: Abandoning passionately held hobbies without explanation
- Feeling trapped: Hopelessness about the future, with statements like “What’s the point?”
- Excessive guilt: Dwelling on past mistakes with inability to self-forgive; harsh self-criticism
- Difficulty concentrating: Making uncharacteristic errors at work or while driving
- Persistent negative self-talk: Calling oneself “failure,” “worthless,” or “a burden” repeatedly
Critical insight: These signs represent patterns, not isolated incidents. Occasional irritability after a bad day is entirely normal. Persistent anger that damages relationships for weeks or months warrants professional attention.
💡 For more information, explore the complete segments of our Mental Wellness Series Overview
The Physical Manifestation: When Emotional Pain Becomes Body Pain
/
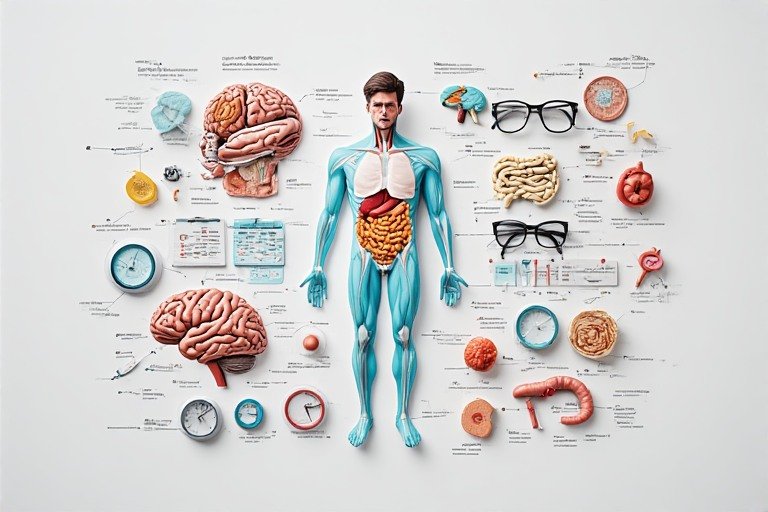
Physical symptoms mapped to body areas: tension headaches (head), chest tightness (heart), stomach issues (gut), back pain (spine), fatigue (whole body)
Men often experience struggles with men’s mental health through physical symptoms—a phenomenon known as somatization. The body expresses what the mind cannot safely articulate, especially when emotional expression feels unsafe or shameful:
Physical Symptom | Emotional Root | When to Seek Help |
| Chest tightness/pressure | Unprocessed stress, anxiety, suppressed anger, or feeling trapped | Always rule out cardiac causes with a physician first; if cardiac causes are excluded, occurrence 3+ times weekly warrants a mental health evaluation |
| Digestive issues (IBS, ulcers) | Gut-brain axis disruption from chronic stress | Persistent despite dietary changes; worsens during stress |
| Back / neck pain | Carrying emotional burden; chronic muscle tension | No clear injury cause; worsens with emotional stressors |
| Persistent fatigue | Depression, burnout, emotional exhaustion | Not improved by rest or vacation time |
| Loss of libido | Stress, depression, emotional disconnection | Affecting relationships or causing significant distress |
The Physical Symptoms of Men’s Mental Health: When Emotional Pain Becomes Body Pain
In the field of men’s mental health, emotional distress often manifests as physical pain—a process called Somatization. The brain redirects psychological tension into the body:
- Chest Pressure: Often linked to acute anxiety.
- Digestive Issues: Driven by the microbiome-mood connection.
- Chronic Back Pain: Caused by long-term muscle tension from suppressed stress.
Critical Insight: Understanding these physical signals is a key step in men’s mental health awareness. When medical tests come back clear but the pain persists, it is time to look at the emotional landscape.
A significant proportion of men presenting with unexplained physical symptoms may have underlying psychological stressors contributing to their condition.
The takeaway: Unexplained physical symptoms warrant both medical evaluation AND mental health consideration. The mind and body are not separate systems. Ignoring the emotional roots of physical symptoms leads to endless doctor visits without resolution.
Redefining Strength: What True Emotional Resilience Looks Like for Men

Society’s definition of male strength is outdated and demonstrably harmful. True emotional resilience looks fundamentally different from what most men were taught:
| Old Definition of Strength (Harmful) | New Definition of Strength (Life-Giving) |
| Never showing vulnerability or uncertainty | Self-awareness: recognizing emotions without judgment |
| Handling everything alone without asking for help | Courage: facing difficult feelings instead of avoiding them |
| Suppressing emotions to maintain “control. “ | Connection: building relationships where vulnerability is safe |
| Never admitting mistakes or personal limitations | Accountability: owning mental health like physical health |
| “Toughing it out” regardless of the cost | Adaptability: adjusting when something isn’t working |
Practical Resilience Builders for Men
- Daily emotional check-in: 2 minutes asking “How am I really doing?” without judgment or performance
- Vulnerability practice: Share one genuine feeling weekly with someone you trust (“I felt overwhelmed today” vs. “I’m fine”)
- Boundary setting: Say no to protect mental energy; stop overcommitting to prove worth
- Help-seeking habit: Normalize asking for support in small ways to build the muscle for bigger asks
The ripple effect: Every man who chooses vulnerability over silence creates permission for others to do the same. Your courage doesn’t just heal you—it gives other men around you permission to heal themselves.
Practical First Steps: How to Start the Conversation (With Yourself or Others)

If You’re Struggling: Starting With Yourself
- Step 1 — Name the feeling without judgment: Instead of “I shouldn’t feel this way,” try “I notice I’m feeling overwhelmed.”
Research on affect labeling shows that putting feelings into words can reduce amygdala activation and emotional intensity.[5] - Step 2 — Write one honest sentence: “I’ve been feeling ______ lately.” No paragraphs needed—one sentence breaks the silence pattern
- Step 3 — Reach out with low stakes: Text a trusted friend: “Having a tough week. Could use a walk Saturday if you’re free.” No pressure to disclose everything immediately
If Supporting Another Man: Creating Safe Entry Points
Instead of: “You seem depressed. You should see a therapist.”
Try: “I’ve noticed you’ve seemed stressed lately. I’m here if you want to talk—no pressure, no judgment.”
Use activity-based connection: men often communicate better side-by-side than face-to-face. Invite him to go for a walk or drive, work on a project together, or exercise. Shared physical activity releases endorphins that ease emotional expression naturally.
Normalize help-seeking by sharing your own experience: “I started seeing a therapist last year for work stress. Honestly, it helped more than I expected.”
What NOT to Do
- Minimize: “Just think positive,” “Man up,” “Everyone has problems.”
- Fix immediately: Jumping to solutions before emotional validation creates resistance
- Force disclosure: Pressuring someone to “open up” before they’re ready backfires
- Keep dangerous secrets: If he mentions self-harm or suicide, contact crisis resources immediately—this is lifesaving, not betrayal
Crisis Resources
- 988 suicide& Crisis Lifeline: Call or text 988 (24/7, free, confidential) [9]
- Crisis Text Line: Text HOME to 741741
- Veterans Crisis Line: Call 988 then press 1, or text 838255 [9]
💡 For more information, explore the complete segments of our Mental Wellness Series Overview
Finding the Right Support: Therapists Who Understand Men’s Experience

Not all therapists understand male socialization or communication styles. Finding the right fit dramatically increases the likelihood of success and sustained engagement:
| Professional | Best For Men With | What to Expect |
| Psychologist (PhD/PsyD) | Depression, anxiety, trauma, and relationship issues | Talk therapy 50 mins/week; evidence-based structured approaches |
| Licensed Clinical Social Worker (LCSW) | Life transitions, family dynamics, practical support | Therapy combined with resource connection is often more affordable |
| Psychiatrist (MD) | Severe depression, bipolar disorder, medication needs | Medical evaluation, prescription management—often combined with therapy |
| Licensed Professional Counselor (LPC) | Stress management, career issues, mild-to-moderate concerns | Skill-building focus; typically more action-oriented approaches |
Finding a Therapist Who Gets Men
- Look for clinicians who specialize in men’s issues or masculinity-informed approaches
- Prefer action-oriented therapies (CBT, ACT, solution-focused) over purely insight-oriented styles
- Check for telehealth options—privacy and convenience significantly increase male engagement
- Search terms: “men’s therapist near me,” “masculinity counseling,” “therapy for men.” Psychology Today: Find a Therapist [11]
Cost Considerations
- Insurance: Most plans now cover mental health (check your deductible and copay)
- Sliding scale: Many therapists offer income-based fees of $40–$100 per session
- Employee Assistance Programs (EAP): Free 3–8 sessions per issue through your employer
- Community mental health centers: Low-cost options based on income level
Investment perspective: Therapy costs less than divorce, job loss, or medical treatment for stress-related illness. It’s healthcare, not a luxury or a sign of weakness.
Building Brotherhood: Creating Safe Spaces for Male Vulnerability

Men thrive in brotherhood—but modern life has progressively eroded traditional male spaces where vulnerability could safely emerge. Rebuilding these connections requires deliberate intention:
| Brotherhood Model | Structure | Why It Works for Men |
| Men’s groups | Weekly or monthly meetings with facilitated sharing | Structured format eliminates the “what do we talk about?” anxiety |
| Activity-based connection | Hiking groups, pickup basketball, and woodworking clubs | Side-by-side interaction lowers the vulnerability barrier significantly |
| Mentorship programs | Older men guiding younger men through life transitions | Provides purpose while building meaningful cross-generational bonds |
| Veterans groups | Shared experience creates immediate, deep trust | Common language around struggle and resilience accelerates connection |
Starting Small: You Don’t Need a Formal Group
- Text 2–3 trusted male friends: “Thinking we should connect more. Coffee this month?”
- Suggest a specific activity: “Hiking Saturday morning? No agenda—just good to catch up.”
- Share one genuine thing when together: “Work’s been tough lately” opens the door for others to do the same
Creating Safety in Male Spaces
- Lead by example: Be the first to share something real—not trauma-dumping, but authentic
- No fixing: Listen without immediately offering solutions; presence matters more than answers
- Confidentiality: What’s shared in the group stays in the group, always
- No judgment: Avoid comments that shame vulnerability, even disguised as humor
Strong social relationships are associated with a significantly reduced risk of premature mortality.[6]
FAQ
Q1: What are the primary barriers to men’s mental health and emotional expression?
Social conditioning often teaches men that vulnerability is a weakness. This “stigma” acts as a major barrier, making it difficult for men to seek help or discuss their internal struggles openly.
Q2: How does anger mask underlying men’s mental health issues like depression?
In many men, depression doesn’t manifest as sadness, but as irritability or rage. This is because anger is often seen as a more “socially acceptable” male emotion than vulnerability or fear.
Q3: When is it time to seek professional support for men’s mental health?
You should consider professional support if symptoms—such as persistent anger, loss of interest, or physical pain—last more than two weeks or begin to interfere with your work and relationships.
Q4: What if therapy doesn’t work for me?
Therapy is not one-size-fits-all. If your first therapist isn’t a good fit, try someone else without giving up on the process. Different approaches (CBT, ACT, psychodynamic) suit different people. Give each therapist 3–4 sessions before deciding, but trust your gut—the therapeutic relationship itself is a major factor in outcomes.
Q5: Can exercise replace therapy for depression?
Meta-analyses show that regular physical activity significantly reduces symptoms of mild to moderate depression (Singh et al., 2023; Kvam et al., 2016). [7][10]. But it’s not a replacement for therapy in moderate-to-severe cases. The strongest approach combines physical activity with professional support for synergistic benefits.
Q6: How do I support a male friend without being pushy?
Express concern once clearly, then give space: “I care about you, and I’m here if you want to talk” is enough. Continue inviting him to activities without pressure or agenda. Consistency matters more than intensity—showing up repeatedly over time builds the trust that eventually opens the door.
Q7: How do men’s mental health symptoms differ from female-pattern depression?
While women often experience “internalizing” symptoms like withdrawal or sadness, men frequently show “externalizing” symptoms, including risk-taking, substance use, or unexplained physical body pain.
Mental Wellness Series Overview
This article is part of the Mental Wellness Series — an evidence-based collection of guides exploring psychological resilience, mental health strategies, and the science behind sustainable wellbeing in 2026.
REFERENCES
- [1] Garnett, M. F., & Curtin, S. C. (2024). Suicide Mortality in the United States, 2002-2022. NCHS Data Brief, No. 509. National Center for Health Statistics, CDC. https://www.cdc.gov/nchs/products/databriefs/db509.htm
- [2] National Institute of Mental Health. (2024). Men and Mental Health. NIMH, U.S. Department of Health and Human Services. (40% of men with mental illness receive treatment vs. 52% women) https://www.nimh.nih.gov/health/topics/men-and-mental-health
- [3] American Psychological Association. (2024). Men and Mental Health: Understanding the Barriers to Treatment Seeking. APA Division 51 (Society for the Psychological Study of Men and Masculinities).
https://www.apa.org/topics/men-masculinity - [4] Griffith, D. M., Bruce, M. A., & Thorpe, R. J. (2024). Men and Mental Health: What Are We Missing? Association of American Medical Colleges. AAMC Analysis.
https://www.aamc.org/news/men-and-mental-health-what-are-we-missing - [5] Lieberman, M. D., Eisenberger, N. I., Crockett, M. J., Tom, S. M., Pfeifer, J. H., & Way, B. M. (2007). Putting feelings into words: Affect labeling disrupts amygdala activity in response to affective stimuli. Psychological Science, 18(5), 421-428. doi:10.1111/j.1467-9280.2007.01916.x https://pubmed.ncbi.nlm.nih.gov/17576282/
- [6] Holt-Lunstad, J., Smith, T. B., Baker, M., Harris, T., & Stephenson, D. (2015). Loneliness and social isolation as risk factors for mortality: A meta-analytic review. Perspectives on Psychological Science, 10(2), 227-237. doi:10.1177/1745691614568352
https://pubmed.ncbi.nlm.nih.gov/25910392/ - [7] Kvam, S., Kleppe, C. L., Nordhus, I. H., & Hovland, A. (2016). Exercise as a treatment for depression: A meta-analysis. Journal of Affective Disorders, 202, 67-86. doi:10.1016/j.jad.2016.03.063 https://pubmed.ncbi.nlm.nih.gov/27253219/
- [9] 988 Suicide and Crisis Lifeline. (2024). For People in Crisis: Resources and Intervention Data. SAMHSA.
https://www.988lifeline.org/ - [10] Singh, B., Olds, T., Curtis, R., et al. (2023). Effectiveness of physical activity interventions for improving depression, anxiety, and distress. British Journal of Sports Medicine, 57(18), 1203-1209. doi:10.1136/bjsports-2022-106195
https://pubmed.ncbi.nlm.nih.gov/36796860/ - [11] Transforming the understanding and treatment of mental illnesses.
https://www.nimh.nih.gov/health/statistics/mental-illness - [12] Psychology Today: Find a Therapist
https://www.psychologytoday.com/us





