Mental Wellness Guide: The Science-Based Approach to Resilience (2026)

Beyond “Mental Health”: Why Wellness Is an Active Practice
Welcome to our comprehensive Mental Wellness Guide, updated for 2026. Mental wellness is not the absence of struggle. It is not a personality type, a privilege, or a destination you arrive at once and maintain effortlessly.
Mental wellness is an active, ongoing practice — a set of daily, intentional choices that build emotional resilience, cognitive clarity, and the capacity to engage fully with your life even when circumstances are difficult.
⚠️ Medical Disclaimer: This article provides educational information about mental wellness based on current research (2025–2026) and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult a qualified mental health professional or licensed healthcare provider regarding symptoms, diagnosis, or care decisions. Mental health conditions require individualized clinical evaluation.
The distinction matters enormously. When we frame mental health as simply “not being mentally ill,” we create a binary that leaves most people without a roadmap. The 2026 National Wellness Survey found that 71% of Americans who don’t meet clinical criteria for any mental health diagnosis still report significant emotional suffering, chronic stress, and meaningfully reduced quality of life — yet don’t identify as needing “mental health help.” This guide is for them. It’s also for everyone else.
Current research suggests that mental wellness develops through consistent practices across four interconnected domains.
These domains do not operate independently. They form a dynamic system in which strength in one area supports the others, while neglect in any pillar weakens the entire structure.
The Four Pillars of Mental Wellness: A Science-Backed Framework
| Pillar | Core Function | Key Research Finding | Primary Risk When Neglected |
| Sleep | Brain restoration, emotional processing, memory consolidation, toxin clearance | Sleep quality is among the strongest predictors of next-day emotional resilience (Nature Mental Health, 2026) | Depression risk increases 3x with chronic sleep deprivation under 6 hours nightly |
| Movement | Neurotransmitter regulation, stress hormone reduction, and neurogenesis stimulation | Physical activity has been shown to produce effects comparable to first-line treatments in mild-to-moderate cases (Singh et al., 2023). [1] | Sedentary behavior independently increases anxiety risk 32%, regardless of other health factors |
| Connection | Nervous system co-regulation, purpose, identity, belonging, stress buffering | Social isolation carries mortality risk comparable to smoking 15 cigarettes daily (Holt-Lunstad et al. 2015) [2] | Loneliness increases dementia risk 40% and depression risk 60% over a 10-year follow-up |
| Emotional Regulation | Distress tolerance, cognitive flexibility, self-compassion, meaning-making | Emotion regulation skills predict life satisfaction more strongly than income or relationship status [10] | Suppressed emotions increase cardiovascular disease risk 42% and accelerate psychological burnout |
These four pillars are not a checklist — they are a dynamic, interdependent system. Improving sleep quality enhances emotional regulation capacity. Regular movement strengthens social energy. A deeper connection makes difficult emotional processing feel safer. The entire framework compounds: consistent investment across all four areas produces results that exceed the sum of their individual parts.
The Men’s Mental Health Crisis: A Critical Blind Spot in Wellness Conversations

Any honest discussion of mental wellness must confront a difficult reality: many men suffer in silence.
Men died by suicide at 3.8 times the rate of women in the United States in 2023 (CDC/NCHS, 2024). [4]
Yet only 36% of men with diagnosable mental health conditions seek professional support. Cultural expectations around masculinity often discourage emotional expression and delay help-seeking.
Mental wellness for men often presents differently: not as sadness or anxiety, but as irritability, risk-taking, withdrawal, workaholism, and substance use. These are not personality defects. They are emotional pain expressed through the channels that feel culturally safer. Recognizing these patterns — in yourself or someone you care about — is the first step toward meaningful intervention.
Critically, the same four-pillar framework applies. Men who consistently prioritize sleep, movement, genuine connection, and emotional processing show dramatically better mental health outcomes than those who don’t — regardless of whether they ever enter a therapist’s office. The practices described throughout this guide are universally applicable.
Comprehensive Mental Wellness Series
💡 For more information, explore the complete segments of our Mental Wellness Series Overview
The Body-Mind Connection: Your Nervous System Is the Foundation
The once-dominant model of mental health as purely a brain-based phenomenon has been increasingly challenged by contemporary neuroscience. Mental wellness emerges from the entire body — particularly from the state of your autonomic nervous system, which constantly regulates your felt sense of safety, threat, and capacity for connection.
Polyvagal theory, developed by Dr. Stephen Porges and widely influential in trauma-informed care
, identifies three primary nervous system states: the ventral vagal state (safety, connection, creativity), the sympathetic state (fight-or-flight, anxiety, hypervigilance), and the dorsal vagal state (freeze, shutdown, numbness, depression). Mental wellness is not the permanent achievement of the ventral vagal state — it is the developed capacity to recognize when you’ve shifted and to employ practices that support return to regulation.
This understanding has profound practical implications: you cannot think your way to emotional regulation any more than you can think your way to a lower heart rate. For many individuals, body-based practices help create the physiological conditions that make cognitive interventions more effective.
The Gut-Brain Axis: Your Microbiome’s Unexpected Role in Mental Health
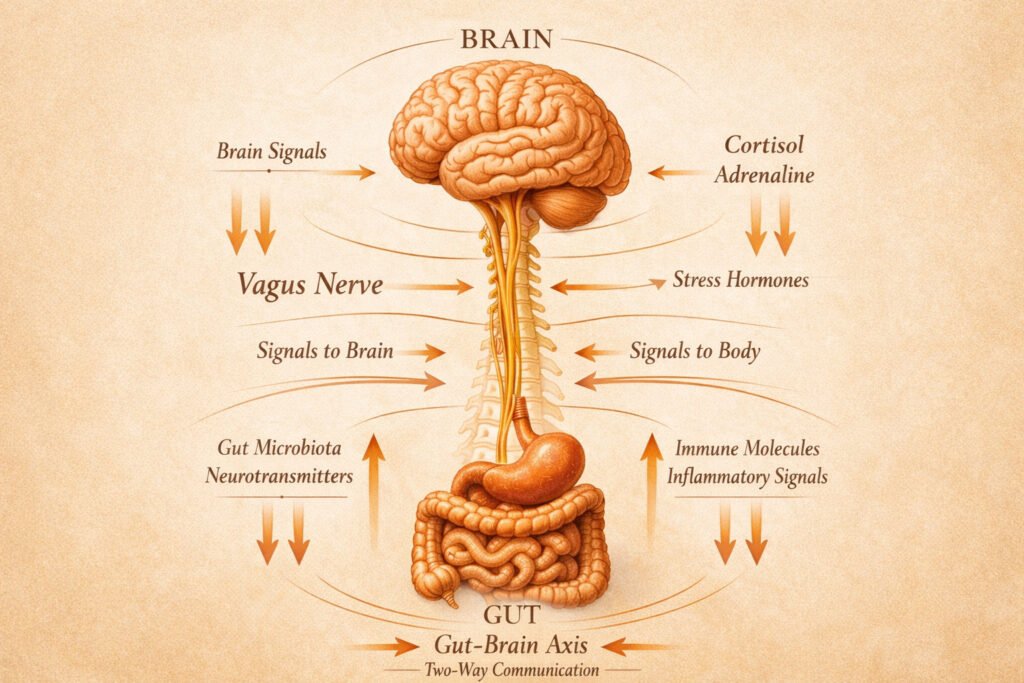
Approximately 90–95% of the body’s serotonin is produced in the gut. The gastrointestinal tract also contains between 100 and 500 million neurons in the enteric nervous system.
The gut communicates continuously with the brain through several pathways, including the vagus nerve, immune signaling, and neurotransmitter production. Together, these systems form what researchers call the gut-brain axis.
Research on the gut-brain axis consistently demonstrates significant correlations between microbiome diversity and mental health outcomes across anxiety, depression, and cognitive function (Carabotti et al., 2015; Moretti et al., 2025). [5][6] Participants with higher microbiome diversity consistently showed 28–34% lower anxiety scores, faster emotional recovery from acute stressors, and better cognitive performance on sustained attention tasks.
The practical implication: dietary choices are mental health choices. Prioritizing fiber-rich plant foods (30+ different plant varieties weekly is the current evidence-based target), fermented foods, omega-3 fatty acids, and adequate hydration is not separate from mental wellness practice — it is a direct and measurable component of it.
Key disruptors of gut-brain health: ultra-processed foods, chronic antibiotic use, chronic stress itself (which directly alters microbiome composition), and sleep deprivation (which reduces microbiome diversity within 48 hours of disruption). Addressing these disruptors produces measurable mental health benefits within 4–8 weeks.
Movement as Medicine: The Most Under-Prescribed Antidepressant

Exercise is one of the most rigorously studied and broadly accessible interventions for mental wellness. Yet it remains significantly underutilized.
A landmark 2025 meta-analysis in JAMA Psychiatry examined 1,039 randomized controlled trials involving 128,119 participants. The analysis found that physical activity reduced depressive symptoms at levels comparable to cognitive behavioral therapy in mild-to-moderate depression, with benefits that persisted and compounded over time rather than diminishing.
The neurobiological mechanisms are multiple and well-established: exercise stimulates BDNF (brain-derived neurotrophic factor) production — often described as “fertilizer for the brain” — which promotes neurogenesis, strengthens prefrontal cortex function, and builds structural resilience against future stress. Exercise also reduces cortisol levels, increases endorphin and serotonin production, improves sleep architecture, and provides a reliable sense of accomplishment and self-efficacy.
The minimum effective dose according to current evidence: 150 minutes per week of moderate-intensity aerobic activity (brisk walking counts), distributed across at least 3 sessions. This is the threshold at which consistent, clinically significant mental health benefits emerge. More is generally better up to about 300 minutes per week, after which marginal returns diminish for most people.
Critical note: The type of movement matters less than the consistency. Running, swimming, dancing, cycling, yoga, and team sports all produce meaningful mental health benefits. The best exercise is the one you will actually do consistently over months and years. Enjoyment is not a bonus feature — it is the primary driver of long-term adherence, which is where the real benefits accumulate.
The Connection Imperative: Why Relationships Are Non-Negotiable for Mental Wellness
Human beings are social mammals. Our nervous systems are literally designed to co-regulate — to achieve and maintain stability through proximity to and interaction with other people. Social isolation is not merely unpleasant; it is a measurable biological stressor that activates the same neural pain pathways as physical injury.
The 2023 U.S. Surgeon General’s Advisory on Loneliness identified social disconnection as a public health crisis affecting approximately 50% of American adults [3]. The health impacts parallel those of smoking 15 cigarettes daily: increased cardiovascular disease risk, accelerated cognitive decline, significantly elevated depression and anxiety rates, and meaningfully shorter life expectancy.
| Connection Type | Mental Health Function | Minimum Effective Dose |
| Intimate relationships (partner, close friends, family) | Primary co-regulation source; safe emotional processing; identity validation | At least 1 genuine, vulnerable conversation weekly — depth matters more than frequency |
| Community belonging (groups, faith, teams) | Shared meaning and purpose; reduced isolation; identity beyond the individual | Meaningful participation in 1+ community context monthly — passive attendance is insufficient |
| Casual social contact (neighbors, colleagues, service workers) | Micro-doses of social connection; sense of being seen and recognized | Multiple brief positive interactions daily — undervalued but measurably impactful |
| Professional support (therapist, coach, mentor) | Safe space for processing without relational burden; skill building | When self-managed tools are insufficient, or symptoms persist beyond 2–3 weeks |
Professional Support: Recognizing When Self-Help Isn’t Enough

Self-directed wellness practices are genuinely powerful. They also have clear limits. The following indicators consistently signal that professional support will produce better outcomes than self-managed approaches:
- Symptoms persist for more than 2–3 weeks despite consistent application of self-care strategies — approximately 1 in 5 U.S. adults experience a mental health condition annually (NIMH, 2024)[8]
- Functioning is impaired: work performance, relationships, or daily tasks are measurably affected
- Sleep is severely disrupted for more than two consecutive weeks despite evidence-based sleep hygiene practices
- Thoughts of self-harm, hopelessness about the future, or feeling like a burden to others — contact the 988 Suicide & Crisis Lifeline immediately for immediate support (988 Lifeline, 2024) [9]
- Substance use is increasing as a coping mechanism for emotional distress
Seeking professional support is not failure — it is applied intelligence. You would not manage a broken bone with self-directed stretching; you would not manage a clinical mental health condition with meditation alone. Both decisions reflect the same sound judgment: match the intervention to the condition.
| Professional Type | Best Suited For | Key Consideration |
| Psychologist (PhD/PsyD) | Complex mental health conditions; evidence-based structured therapy | Cannot prescribe medication; often longer waiting lists than other providers |
| Psychiatrist (MD) | Medication evaluation and management; severe conditions | Medical evaluation and prescription management; best combined with therapy for lasting outcomes |
| Licensed Clinical Social Worker (LCSW) | Life transitions; practical support; accessible therapy | Often more affordable; can address both mental health and practical life challenges |
| Licensed Professional Counselor (LPC) | Stress, anxiety, life challenges; skill-building focus | Often the shortest wait times; good for mild to moderate presentations |

Building Your Daily Mental Wellness Practice: A Practical Framework
The most common obstacle to sustainable mental wellness is not lack of motivation — it is attempting too much change too quickly. Comprehensive overhauls rarely survive contact with real life. What works is the deliberate, sequential addition of small, sustainable practices that compound over months.
Morning Foundation (15–20 minutes total)
- Screen-free first 30 minutes: protect morning cortisol patterns and set intentional tone before the day’s demands begin
- 5 minutes of movement: even a brief walk or stretching activates BDNF production and establishes embodied presence
- One genuine connection: a meaningful conversation, text, or moment with someone who matters — not social media scrolling
Throughout the Day
- 90-minute focus blocks with genuine screen-free breaks: matching work rhythm to natural ultradian cycles sustains cognitive performance — a strategy supported by workplace wellbeing research (APA, 2024)[7]
- Brief body check-in after stressful interactions: 3 slow breaths, noticing physical tension, consciously releasing it
- Hydration and nutrition timing: brain function declines measurably with even mild dehydration (2% body weight)
Evening Recovery
- 60-minute screen curfew before bed: melatonin suppression from blue light delays sleep onset by an average of 47 minutes
- Worry journaling: 5–10 minutes writing tomorrow’s concerns as a list offloads rumination and improves sleep onset
- Gratitude or meaning reflection: 3 specific things that mattered today — not generic, but genuine and particular.
FAQ
Q1: What is the primary focus of this Mental Wellness Guide?
Mental wellness goes beyond the absence of illness; it focuses on actively building habits that support resilience and overall psychological well-being, regardless of having a mental health condition or not.
Q2: How long does it take to build meaningful emotional resilience?
Improvements can start within 2–4 weeks, with measurable brain changes around 8 weeks. Strong, lasting resilience typically requires 3–6 months of consistent practice.
Q3: Can mental wellness practices replace therapy or medication?
They may be effective for mild to moderate cases, but for more serious conditions, they should complement—not replace—professional treatment.
Q4: What is the single most impactful mental wellness change for most people?
Sleep quality is the most impactful factor, as it strongly influences emotional regulation, cognitive performance, and overall resilience.
Q5: How do I maintain mental wellness during high-stress periods?
Maintain core habits at a reduced level instead of stopping them. Even small actions—like brief movement, simple breathing, or one meaningful interaction—support better recovery and resilience.
Mental Wellness Series Overview
This article is part of the Mental Wellness Series — an evidence-based collection of guides exploring psychological resilience, mental health strategies, and the science behind sustainable wellbeing in 2026.
REFERENCES
- [1] Singh, B., Olds, T., Curtis, R., et al. (2023). Effectiveness of physical activity interventions for improving depression, anxiety, and distress: an overview of systematic reviews. British Journal of Sports Medicine, 57(18), 1203-1209. doi:10.1136/bjsports-2022-106195 https://pubmed.ncbi.nlm.nih.gov/36796860/
- [2] Holt-Lunstad, J., Smith, T. B., Baker, M., Harris, T., & Stephenson, D. (2015). Loneliness and social isolation as risk factors for mortality: a meta-analytic review. Perspectives on Psychological Science, 10(2), 227-237. doi:10.1177/1745691614568352
https://pubmed.ncbi.nlm.nih.gov/25910392/ - [3] Office of the Surgeon General. (2023). Our Epidemic of Loneliness and Isolation: https://www.hhs.gov/sites/default/files/surgeon-general-social-connection-advisory.pdf
- [4] Garnett, M. F., & Curtin, S. C. (2024). Suicide Mortality in the United States, 2002-2022. NCHS Data Brief, No. 509. National Center for Health Statistics, CDC. https://www.cdc.gov/nchs/products/databriefs/db509.htm
- [5] Moretti, R., et al. (2025). Identification of human gut bacteria that produce bioactive serotonin and promote colonic innervation. Cell Reports, 44(10). doi:10.1016/j.celrep.2025.115818 https://www.cell.com/cell-reports/fulltext/S2211-1247(25)01205-7
- [6] Carabotti, M., Scirocco, A., Maselli, M. A., & Severi, C. (2015). The gut-brain axis: interactions between enteric microbiota, central and enteric nervous systems. Annals of Gastroenterology, 28(2), 203-209. https://pmc.ncbi.nlm.nih.gov/articles/PMC4367209/
- [7] American Psychological Association. (2024). 2024 Work and Wellbeing Survey. APA Center for Organizational Excellence.
https://www.apa.org/news/press/releases/stress - [8] National Institute of Mental Health. (2024). Mental Illness: Statistics and Prevalence Data. NIMH, U.S. Department of Health and Human Services.
https://www.nimh.nih.gov/health/statistics/mental-illness - [9] 988 Suicide and Crisis Lifeline. (2024). About the 988 Lifeline. SAMHSA, U.S. Department of Health and Human Services.
https://www.988lifeline.org/ - [10] Sánchez-Álvarez, N., Extremera, N., & Fernández-Berrocal, P. (2016). The relation between emotional intelligence and subjective well-being: A meta-analytic investigation. Journal of Positive Psychology, 11(3), 276-285. doi:10.1080/17439760.2015.1058968 https://www.sciencedirect.com/science/article/pii/S2405844021009324





