Alzheimer’s Disease: Essential 2026 Guide to Symptoms and Care
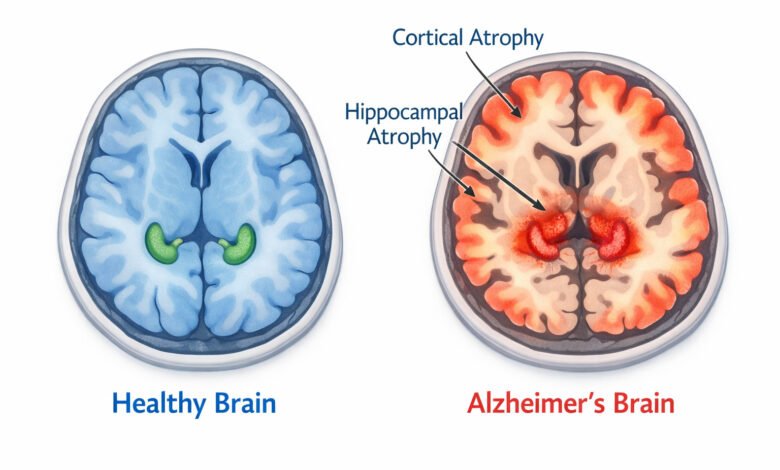
Understanding Alzheimer’s: More Than “Normal Aging”
As part of our [Mental Wellness Guide], we explore how Alzheimer’s disease not only impairs memory but it also progressively alters cognition, behavior, and functional independence, profoundly affecting both patients and families.
Alzheimer’s disease is not a normal part of aging—it’s a progressive neurodegenerative disorder that gradually destroys memory, thinking skills, and the ability to perform everyday tasks. While occasional forgetfulness is a normal part of aging, Alzheimer’s disease involves persistent and worsening patterns that interfere with independence.
⚠️ Medical Disclaimer: This article provides educational information about Alzheimer’s disease based on current research (2025–2026) and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult a qualified neurologist or healthcare professional regarding symptoms, diagnosis, or care decisions. Alzheimer’s disease management requires individualized medical evaluation
According to the Alzheimer’s Association 2025 Facts and Figures report, approximately 6.9 million Americans aged 65+ live with Alzheimer’s Disease today—a number projected to rise to nearly 13 million by 2050. Yet awareness remains dangerously low: Approximately one in three older adults dies with Alzheimer’s disease or another form of dementia, yet only 55% of those affected receive a formal diagnosis.
The critical distinction: Normal aging might mean taking longer to recall a word. Alzheimer’s Disease means forgetting what the word represents entirely—and losing the ability to form new memories to replace it.
Pathological changes in the brain: Plaques, Tangles, and Neuron Loss
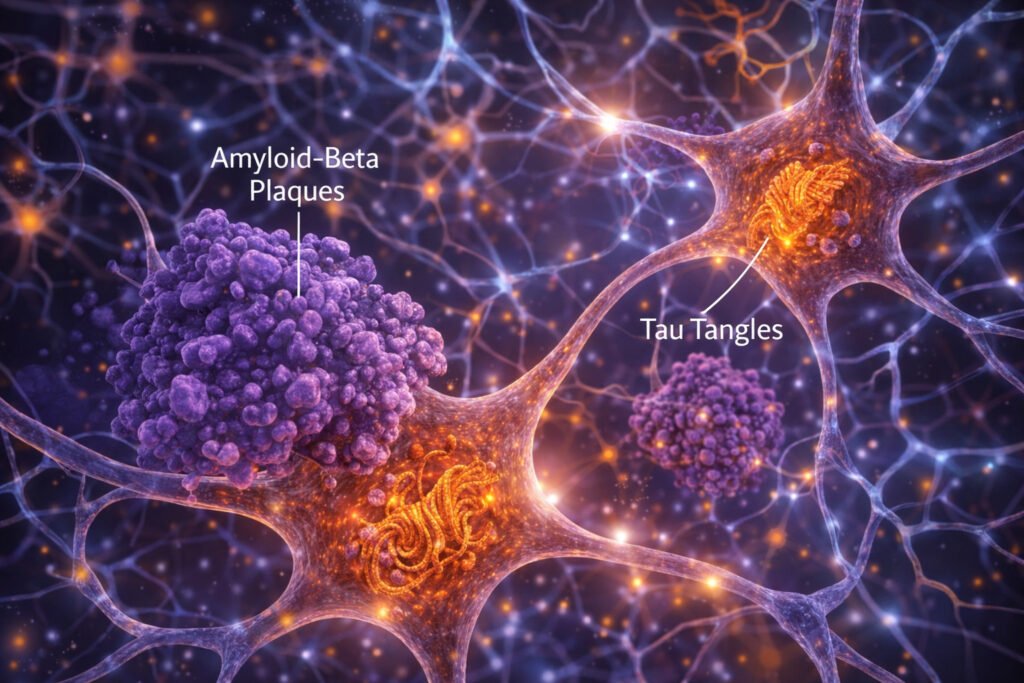
Alzheimer’s disease pathology centers on two abnormal protein structures that disrupt brain communication:
Amyloid-beta plaques form when protein fragments clump together between nerve cells, blocking signals and triggering inflammation. Think of them as “gunk” clogging the brain’s communication highways.
Neurofibrillary tangles develop when tau proteins—normally stabilizing neuron structure—become twisted and collapse the cell’s transport system. This starves neurons of nutrients until they die.
These processes begin 10–20 years before symptoms appear. By the time memory lapses become noticeable, significant brain damage has already occurred—particularly in the hippocampus (memory center) and cortex (thinking/planning regions).
Emerging research is exploring possible links between the gut microbiome and neuroinflammation in Alzheimer’s disease, although causality has not been established. —suggesting the gut-brain axis may play a protective role worth exploring through diet and lifestyle.
Early Warning Signs Most People Miss (Before Memory Loss)

Memory loss gets attention, but these pre-memory symptoms often appear first—and are frequently dismissed:
| Subtle Sign | What It Looks Like | Why It Matters |
| Word-finding difficulty | Pausing mid-sentence, substituting “thing” for specific nouns | Early disruption of language-processing networks in the temporal lobe. |
| Poor judgment | Falling for obvious scams, neglecting finances | Prefrontal cortex deterioration affects decision-making and impulse control early in disease progression |
| Loss of initiative | Abandoning hobbies once enjoyed without explanation | Motivation circuits affected before memory fails |
| Spatial confusion | Getting lost in familiar neighborhoods | Visual processing areas deteriorate early |
| Personality shifts | Uncharacteristic irritability, suspicion, or apathy | Emotional regulation networks are disrupted |
Critical insight: These changes represent patterns, not isolated incidents. Forgetting where you parked once is normal. Forgetting where you parked three times in one week at a familiar location warrants medical evaluation.
The 7 Stages Framework: What to Expect at Each Phase
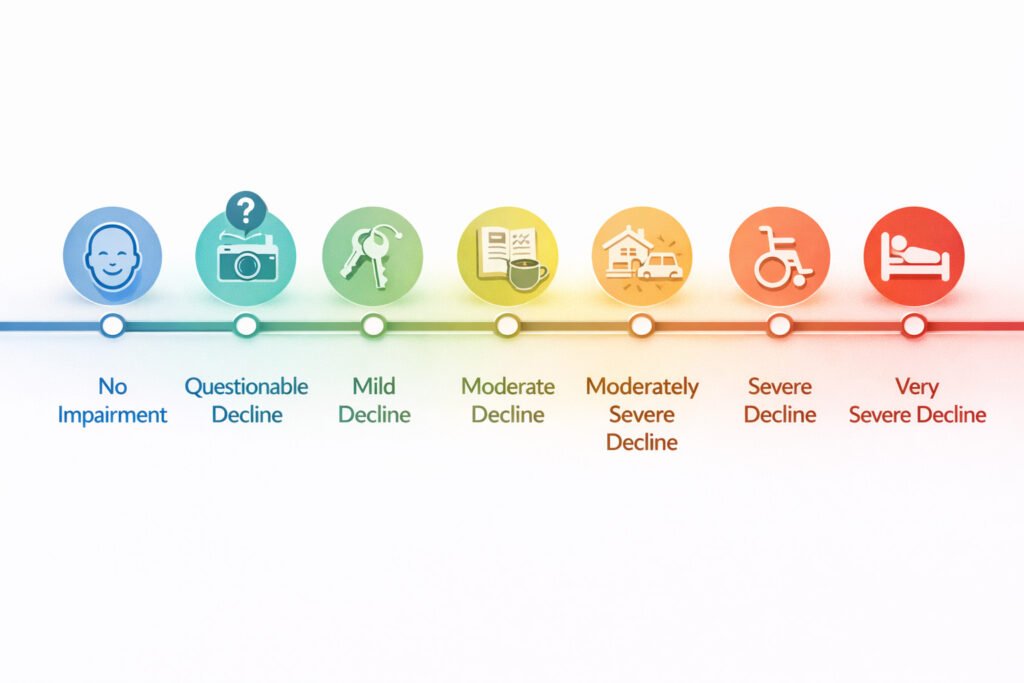
While Alzheimer’s progression varies individually, the Global Deterioration Scale (GDS) provides a practical framework for families and caregivers:
| Stage | Description | Key Characteristics | Recommended Actions |
| Stage 1–2 | No / Very Mild Impairment | No noticeable symptoms; brain changes may be detectable via biomarkers | Focus on prevention: cardiovascular health, sleep quality, cognitive engagement |
| Stage 3 | Mild Cognitive Decline | Word-finding issues, losing items frequently, and decreased work performance | Medical evaluation; establish legal and financial plans while capacity is intact |
| Stage 4 | Moderate Cognitive Decline | Forgets recent events, struggles with complex tasks (managing finances) | Simplify home environment; introduce medication management systems |
| Stage 5 | Moderately Severe Decline | Needs help with daily activities (dressing appropriately), and forgets personal history | Increase supervision; evaluate living arrangements for safety |
| Stage 6 | Severe Decline | Requires help with basic self-care (bathing, toileting); personality changes | Professional caregiving support essential; focus on comfort and dignity |
| Stage 7 | Very Severe Decline | Loses ability to speak, walk, or control movement; requires 24/7 care | Palliative focus: pain management, sensory comfort, family presence |
Important nuance: Progression speed varies widely. Some individuals move through all stages in 4 years; others take 20+. Early diagnosis allows earlier intervention, which may modestly slow functional decline in eligible patients.
💡 For more information, explore the complete segments of our Mental Wellness Series Overview
Risk Factors Within Your Control (and Those Beyond It)
| Non-Modifiable Risks (Beyond Your Control) | Modifiable Risks (Evidence-Based & Within Control) |
|---|---|
| Age: Risk doubles every 5 years after age 65. | Cardiovascular Health: Hypertension, diabetes, and obesity increase risk by 2–3x. |
| Genetics: APOE-e4 variant increases susceptibility but doesn’t guarantee onset. | Physical Inactivity: A sedentary lifestyle increases risk by 30–50%. |
| Family History: Having a first-degree relative with Alzheimer’s increases baseline risk | Sleep Quality: Chronic disruption accelerates amyloid plaque buildup in the brain. |
| Down Syndrome: Nearly universal Alzheimer’s pathology typically develops by the 40s. | Social Isolation: Loneliness increases dementia risk at a rate comparable to smoking. |
| Biological Sex: Women are at a higher risk, partly due to longer life expectancy. | Diet Quality: Mediterranean-style patterns are associated with a 30% lower risk. |
Table 1: Comparison of modifiable and non-modifiable Alzheimer’s risk factors based on 2024-2026 research.
A landmark 2024 Lancet Commission report concluded that addressing 12 modifiable risk factors could prevent or delay up to 40% of dementia cases worldwide—making lifestyle intervention one of the most important strategies currently available.
Diagnosis: Beyond Memory Tests to Advanced Biomarkers

Diagnosis requires ruling out reversible causes (vitamin deficiencies, thyroid issues, medication side effects) through a comprehensive evaluation process:
- Clinical evaluation: Detailed history from patient and family observer (crucial—patients often lack insight into their own decline)
- Cognitive screening: MoCA (Montreal Cognitive Assessment) detects mild impairment better than the older MMSE test
- Blood biomarkers (2026 advances): Plasma p-tau217 testing has demonstrated high diagnostic accuracy in research settings, with performance comparable to amyloid PET in some cohorts for detecting Alzheimer’s pathology (Palmqvist et al., 2024). [4]
- MRI: Rules out tumors and strokes; measures hippocampal shrinkage over time
- Amyloid PET: Visualizes plaque buildup directly (expensive but definitive for diagnosis)
- FDG-PET: Shows metabolic activity patterns characteristic of Alzheimer’s disease vs. other dementias
Critical reality: Many primary care physicians lack specialized dementia diagnostic training. Seek evaluation at a memory disorders clinic or academic medical center for the most accurate diagnosis and access to emerging treatments.
Treatment Options in 2026: Medications, Lifestyle, and Emerging Therapies
FDA-Approved Medications (Symptom Management)
| Medication Class | Examples | How It Works | Limitations |
| Cholinesterase Inhibitors | Donepezil, Rivastigmine | Boosts acetylcholine (memory neurotransmitter) | Modest benefit; does not stop disease progression |
| NMDA Antagonist | Memantine | Regulates glutamate to protect neurons from excitotoxicity | Best for moderate-to-severe stages only |
| Anti-Amyloid Monoclonals | Lecanemab, Donanemab | Removes amyloid plaques from brain tissue and reduces plaque burden as measured by PET imaging | Modest slowing of decline. | Modest slowing of decline; IV infusions required; ARIA side effect risk |
Important context: These medications manage symptoms or modestly slow decline—they do not cure or reverse Alzheimer’s. Benefits are typically measured in months of preserved function, not years.
Lifestyle Interventions with Strong Evidence
- Aerobic exercise: 150 mins/week of brisk walking is associated with reduced cognitive decline risk (Iso-Markku et al., 2024). [5]
- Mediterranean-DASH diet: Emphasizes vegetables, berries, nuts, olive oil, and fatty fish for neuroprotection
- Cognitive stimulation: Structured activities (not passive TV) maintain neural connections longer
- Sleep optimization: 7–8 hours nightly supports the glymphatic system (brain’s waste-clearing process)
Emerging Therapies to Watch
- Multi-domain interventions: Combining diet, exercise, cognitive training, and vascular risk management (based on FINGER trial model)
- Gut microbiome modulation: Early research on probiotics and prebiotics for neuroinflammation reduction
- Precision medicine approaches: Tailoring treatments based on individual genetic and biomarker profiles
Caution: Avoid unproven “cures”—coconut oil, high-dose supplements, and unregulated peptides lack robust evidence and may cause harm or dangerous medication interactions. Always discuss new treatments with a neurologist.
The Caregiver’s Role: Practical Support Strategies That Actually Help

Caregiving for individuals with Alzheimer’s disease is associated with significant physical and psychological stress. Evidence-based strategies that preserve dignity while managing day-to-day challenges:
Communication Techniques
- Use simple, one-step directions (“Please sit here,” not “Come sit down so we can eat lunch together”)
- Avoid arguing about reality—validate emotion instead: “You miss Dad. Tell me about him.”
- Maintain eye contact at their level; touch their arm gently before speaking to gain attention
- Offer choices between two options only: “Red shirt or blue shirt?”, not open-ended questions
Environmental Modifications
- Remove tripping hazards; install grab bars in bathroom (installing grab bars and removing tripping hazards significantly reduces fall risk.)
- Use contrasting colors (white plate on dark table) to improve food visibility and independence
- Label cabinets with pictures and words to help maintain independence longer during disease progression.
Self-Care for Caregivers
Respite care isn’t selfish—it’s essential. Burnout harms both caregiver and care recipient. Research shows caregiving can increase both stress levels and long-term health risks for caregivers. (American Journal of Geriatric Psychiatry, 2025).[6] Join evidence-based programs like REACH II (Resources for Enhancing Alzheimer’s disease Caregiver Health) and monitor your own health consistently.
In summary:
Alzheimer’s disease challenges one of the most fundamental aspects of human life: memory, identity, and independence. As research continues to reveal the biological mechanisms behind the disease—from amyloid plaques and tau tangles to complex interactions involving genetics, lifestyle, and brain health—it becomes increasingly clear that early awareness and proactive care are essential.
Recognizing subtle cognitive changes, seeking timely medical evaluation, and adopting protective lifestyle habits can make a meaningful difference in how the disease unfolds. Advances in diagnostic biomarkers and emerging therapies are gradually transforming the clinical landscape, offering earlier detection and modest but important improvements in disease management.
Equally important is the human dimension. Families and caregivers play a critical role in maintaining dignity, safety, and emotional connection throughout the progression of the illness. Support systems, practical caregiving strategies, and informed medical guidance can significantly improve the quality of life for both patients and those who care for them.
Although Alzheimer’s disease remains one of the most complex neurological challenges of our time, growing scientific knowledge and compassionate care approaches are steadily reshaping how society responds to it—moving the conversation from fear and misunderstanding toward earlier action, better support, and continued hope for more effective treatments in the future.
FAQ
Q1: Is Alzheimer’s disease hereditary?
Having a parent with Alzheimer’s disease increases your risk approximately 2–4x, but most cases are not directly inherited. The APOE-e4 gene variant increases risk but doesn’t guarantee disease—many people with the variant never develop Alzheimer’s, and many without it do develop the condition.
Q2: Can Alzheimer’s disease be prevented?
No guaranteed prevention exists, but addressing modifiable risk factors—cardiovascular health, physical activity, diet quality, sleep, and social engagement—may delay onset or slow progression in susceptible individuals. The 2026 Lancet Commission estimates up to 40% of cases could be prevented or delayed through lifestyle changes.
Q3: Do brain games or apps prevent Alzheimer’s?
Evidence is limited. General cognitive engagement, such as reading, learning instruments, and social interaction, shows stronger protective effects than isolated “brain training” apps. Novelty and social connection matter more than repetitive digital puzzles.
Q4: Why do people with Alzheimer’s disease repeat questions?
Short-term memory loss prevents them from recalling that they have already asked. Respond each time patiently—arguing or saying “I just told you!” increases agitation without helping. Brief, calm answers work best and preserve the emotional connection.
Q5: When should someone with Alzheimer’s disease stop driving?
Warning signs include: getting lost on familiar routes, slow reaction times, confusing the pedals, and recent traffic violations. Most states require physician reporting of dementia diagnoses. Address this early while the person can still participate in the decision-making process.
Q6: Are vitamins or supplements helpful for Alzheimer’s?
No strong evidence supports high-dose vitamin E, B vitamins, or omega-3s for treating Alzheimer’s. A balanced whole-food diet provides sufficient nutrients. Always discuss supplements with a physician—some interact with prescribed medications and may cause harm.
Mental Wellness Series Overview
This article is part of the Mental Wellness Series — an evidence-based collection of guides exploring psychological resilience, mental health strategies, and the science behind sustainable wellbeing in 2026.
REFERENCES
- [1] Alzheimer’s Association. (2025). 2025 Alzheimer’s Disease Facts and Figures. Alzheimer’s & Dementia, 21(4), e70235. doi:10.1002/alz.70235
https://pmc.ncbi.nlm.nih.gov/articles/PMC12040760 - [2] Cryan, J. F., O’Riordan, K. J., Sandhu, K., Peterson, V., & Dinan, T. G. (2020). The gut microbiome in neurological disorders. The Lancet Neurology, 19(2), 179-194. doi:10.1016/S1474-4422(19)30356-4 https://pubmed.ncbi.nlm.nih.gov/31813933/
- [3] Livingston, G., Huntley, J., Liu, K. Y., et al. (2024). Dementia prevention, intervention, and care: 2024 report of the Lancet standing Commission. The Lancet, 404(10452), 572-628. doi:10.1016/S0140-6736(24)01296-0
https://pubmed.ncbi.nlm.nih.gov/39096926/ - [4] Palmqvist, S., Tideman, P., Mattsson-Carlgren, N., et al. (2024). Blood biomarkers to detect Alzheimer’s disease in primary care and secondary care. JAMA, 332(15), 1245-1257. doi:10.1001/jama.2024.13855
https://pubmed.ncbi.nlm.nih.gov/39068545/ - [5] Iso-Markku, P., Aaltonen, S., Halme, H. L., et al. (2024). Physical activity and cognitive decline among older adults: a systematic review and meta-analysis. JAMA Network Open, 7(2), e2354285. doi:10.1001/jamanetworkopen. 2023.54285
https://pmc.ncbi.nlm.nih.gov/articles/PMC10835510/ - [6] Schulz, R., & Sherwood, P. R. (2008). Physical and mental health effects of family caregiving.American Journal of Nursing, 108(9 Suppl), 23-27. doi:10.1097/01.NAJ.0000336406.45248.4c
https://pmc.ncbi.nlm.nih.gov/articles/PMC2791523/ - [7] National Institute on Aging. (2024). Alzheimer’s Disease Fact Sheet. U.S. Department of Health and Human Services.
https://www.nia.nih.gov/health/alzheimers-disease-fact-sheet - [8] Resources for Enhancing Alzheimer’s disease Caregiver Health (REACH) Project https://www.ajgponline.org/article/S1064-7481(12)61775-8/abstract





